Authors:
Jesus Peteiro* and Alberto Bouzas-Mosquera
Department of Cardiology, Complejo Hospitalario Universitario de A Coruña (CHUAC), University of A Coruña, A Coruña, Spain
Received: October 12, 2014; Accepted: October 15, 2014; Published: October 17, 2014
Jesus Peteiro, P/Ronda 5-4º izda.15011-A Coruña, Spain, Fax: 34-81-178001; Email:
Peteiro J, Bouzas-Mosquera A (2014) Exercise Echocardiography in Hypertrophic Cardiomyopathy. J Cardiovasc Med Cardiol 1(2): 035-037. 10.17352/2455-2976.000009
© 2014 Peteiro J, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Hypertrophic cardiomyopathy (HCM) is a relatively frequent genetic disease that affects 1/500 human beings. Main problems with this disease are the development of symptoms in 10-20% of affected individuals, and the increased risk of sudden cardiac death (SCD) in a subset of patients with the disease. It is important to clarify the cause of symptoms and to assess the risk of sudden death in HCM because we do have therapies to relief these problems.
Main causes of symptoms in HCM are related to either LV outflow tract or mid ventricular obstruction, LV diastolic dysfunction, and myocardial ischemia. Drug refractory heart failure symptoms due to LV obstruction may be successfully treated by septal myotomy-myectomy. Alcohol septal ablation or dual-chamber pacemaker are reserved as alternatives to surgery. Indeed, exercise may have a role in discerning the role of LV obstruction as a cause of symptoms in these patients. A comprehensive exercise echocardiography approach can discover a truly symptomatic status in minimally symptomatic or asymptomatic patients, as well as measure LV obstruction, mitral regurgitation (MR) and global and regional wall motion response to exercise (Figures 1 and 2). Recent guidelines recognize exercise echocardiography as a safe and important adjunct in the management of HCM [1]. LV obstruction may develop only during exercise, and it is frequently associated to mitral regurgitation with the typical jet directed posterior as if it were a mitral valve septal prolapse jet. Although LV obstruction during or immediately after exercise can be easily measured by continuous wave Doppler, quantitative assessment of mitral regurgitation by the proximal isovelocity area (PISA) method is commonly difficult as the mitral regurgitation signal is mixed with the LV outflow tract aliasing jet. LV obstruction can be assessed be during a treadmill exercise study in the standing position, or during a bicycle exercise study. It is important to take into account that measurements post-exercise, particularly in the upright position, would give higher values [2] as preload decreases significantly a few seconds after ceasing the lower limbs muscular activity. However, these assessments are real and may correlate with clinical symptoms. Up to 60% of symptomatic patients without resting obstruction (<30 mmHg) may have LV obstruction during an exercise echocardiography study [3]. In contrast, in a recent work, patients who experienced a decrease in LV gradients during exercise had better functional class and a trend to better outcome than those who had increase or no change in their gradients [4]. Indeed there are not plausible alternatives to exercise echocardiography for studying patients with HCM as pharmacological stress with dobutamine may induce the appearance of LV gradients even in normal subjects.
-
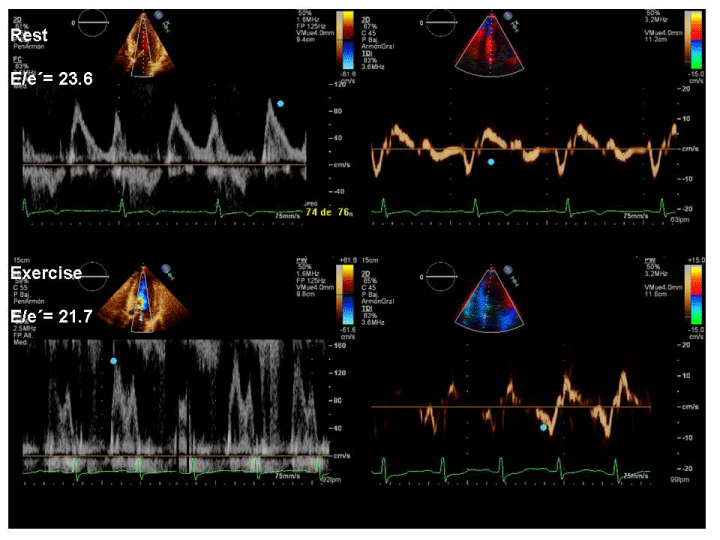
Figure 2
Pulsed Doppler LV inflow and tissue Doppler mitral annulus waves at rest and at exercise. Both resting and exercise E/e´ ratios were increased.
The risk of SCD is not easily predictable in HCM. Therefore several risk factors have been proposed in an approach similar to that for patients with coronary artery disease, to help decisions regarding defibrillator implantation, namely a personal history of malignant arrhythmias, a family history for SCD events, unexplained syncope, documented non-sustained ventricular tachycardia, severe hypertrophy and abnormal blood pressure during exercise. An obstructive left ventricle outflow tract (LVOT) gradient at rest or during provocation, a LV apical aneurysm, late gadolinium enhancement (LGE) by magnetic resonance and specific sarcomeric mutations are currently considered as potential SCD risk modifiers [1].
Exercise echocardiography might also have a role for predicting outcome in patients with HCM. In a recent study of our institution we performed treadmill exercise echocardiography studies in 239 consecutive patients with HCM [5]. LV obstruction and MR were measured immediately after exercise, whereas LV function was assessed during peak exercise. LVOT obstruction at rest was seen in 60 patients (25%), and 43 (18%) developed exercise-induced LVOT obstruction. Mean resting LVEF was 69±9%. We found exercise-induced wall motion abnormalities (WMAs) in 19 patients (7.9%). During a follow-up of 4.1±2.6 years, 19 patients had hard events (cardiac death, cardiac transplantation, appropriate discharge of a defibrillator, stroke, myocardial infarction, or hospitalization due to heart failure) and 41 patients had composite endpoints of hard or soft events (including atrial fibrillation and syncope). Exercise WMAs were more frequent in patients with hard events than in those without (31.5% vs. 5.9%, p<0.001). After adjustment, LV wall thickness (hazard ratio [HR], 1.13; 95% confidence interval [CI], 1.05–1.21; P = .002), resting wall motion score index (HR, 21.59; 95% CI, 2.38–196.1, P = .006), and exercise workload in metabolic equivalents (HR, 0.74; 95% CI, 0.63–0.88; P = .001) remained independent predictors of hard events. Change in wall motion score index was also independently associated with hard events (HR, 52.30; 95% CI, 3.81–718.5; P = .003) and with the composite end point (HR, 39.51; 95% CI, 3.79–412.4; P = .002). Interestingly LV outflow tract obstruction was not associated with either endpoint. In another also recently published study in patients with HCM submitted to exercise echocardiography, predictors of outcome were achieved METs, heart rate recovery and presence of atrial fibrillation, but not LV outflow tract response [6].
The relationship between exercise-induced wall motion abnormalities and myocardial fibrosis by late gadolinium enhancement (LGE) in HCM was further explored by our group. We found that there is an association as exercise wall motion score index correlated with myocardial mass with LGE (r=0.20, p=0.02) and with perfusion defect area (r=0.40, p<0.001). An extensive LGE signal (≥15% of the LV myocardium) was observed more frequently in patients with exercise wall motion abnormalities than in those without (38% vs. 12% without, p=0.009) likely reflecting the lack of contractile reserve in fibrotic myocardium (unpublished data) [7].
Therefore, exercise echocardiography is a reliable and safe technique to measure important variables in HCM. The decision making process can vary should significant LV obstruction and/or MR regurgitation are found during exercise. Also, exercise derived variables such as maximal achieved exercise workload and exercise-induced wall motion abnormalities may influence prognosis.









Figure 1
On the left, resting and peak exercise images in the 4- and 2-chamber apical views in a patient with HCM and dyspnea during physical effort, at diastole (D) and end-systole (S). Note the reduction of LV cavity with exercise in this patient. LV ejection fraction increased from 64 to 72%. On the right, color and continuous wave Doppler images at rest and at exercise. Note the exercise-induced LV outflow tract obstruction and accompanying mild-to-moderate mitral regurgitation, both due to systolic anterior motion of the mitral valve.
Figure 1: On the left, resting and peak exercise images in the 4- and 2-chamber apical views in a patient with HCM and dyspnea during physical effort, at diastole (D) and end-systole (S). Note the reduction of LV cavity with exercise in this patient. LV ejection fraction increased from 64 to 72%. On the right, color and continuous wave Doppler images at rest and at exercise. Note the exercise-induced LV outflow tract obstruction and accompanying mild-to-moderate mitral regurgitation, both due to systolic anterior motion of the mitral valve.