Author(s):
Blake R. Busey, Rebecca J. Caro* and Dana R. Nguyen
Department of Family Medicine, Family Medicine Residency Clinic, Womack Army Medical Center, Fort Bragg, NC 28310, USA
Received: 30 July, 2014; Accepted: 08 September, 2014; Published: 10 September, 2014
CPT Rebecca J. Caro, Department of Family Medicine, Family Medicine Residency Clinic, Womack Army Medical Center, Fort Bragg, NC 28310, USA, Email:
Busey BR, Caro RJ, Nguyen DR (2015) Primary Amenorrhea: A Müllerian Agenesis Case Report. Global J Med Clin Case Reports 2(1): 007-009. DOI: 10.17352/2455-5282.000010
© 2015 Busey BR, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Primary amenorrhea; Müllerian agenesis; Mayer-Rokitansky-Küester-Hauser Syndrome; MRKH; Blind pouch
A case of müllerian agenesis, Mayer-Rokitansky-Küster-Hauser (MRKH) Syndrome, in a 16 year-old female with primary amenorrhea is reported. This patient exhibited normal female external physical characteristics with a shallow, blind vaginal pouch upon examination. Serologic hormone evaluation as well as karyotype determination revealed normal pubertal female range hormones and 46, XX, respectively. MRKH Syndrome has a prevalence of 1 in 4000 to 10000 females. Treatment is multi-factorial and should include nonsurgical vaginal dilator therapy, surgical neovaginal options, as well as psychosocial support and counseling on future reproductive options.
Case Presentation
A 16 year-old sexually active female with thelarche at 12 years-old and pubarche at 13 years-old presented with primary amenorrhea. She stated that she had bloating, irritability, and low abdominal cramping every 28 days, lasting 1-2 days, without vaginal spotting or bleeding. She stated that she had been sexually active for the last year with the same partner, but she had pain and resistance during attempted intercourse. She also stated that she had vaginal spotting following intercourse.
A review of the patient's past medical history, medications and supplements, allergies, and social history were unremarkable. Her surgical history included an exploratory laparoscopy for suspected appendicitis that proved negative, but a paraovarian cyst was excised with ovarian cyst confirmed (Figure 1). Her family history was unremarkable and no birth defects, sexual anomalies, or chromosomal anomalies were reported.
The physical examination revealed Tanner stage 5 breast development and female pubic hair distribution. A bimanual examination and subsequent speculum examination revealed a blind vaginal pouch approximately 2.5 cm in depth as well as an anterior recess just proximal to the pubic rim. Exploration with a sterile probe revealed that the recess was approximately 6 cm long.
Laboratory results (β-HCG, TSH, LH, FSH, progesterone, prolactin, estradiol, and free and total testosterone) confirmed normal reproductive female hormone levels as well as 46, XX karyotype. Magnetic resonance imaging (MRI) with and without contrast revealed no uterine structures, but ovarian tissue was present (Figures 2-5). The 6 cm vaginal recess was not clearly defined with MRI. Urologic and vaginal structures were re-examined under general anesthesia with cystoscopy and vaginoscopy that revealed a dilated urethral meatus without anomalous renal or urethral structures.
After consultation with a multidisciplinary team (OB/GYN, Reproductive Endocrinology and Infertility, and Urology), the final diagnosis of müllerian agenesis was reached. Our patient was started on progressive vaginal dilator therapy. She is also undergoing counseling regarding her diagnosis and the subsequent emotional burden with the support of her family and friends.
Discussion
Primary amenorrhea is defined as failure to reach menarche. Evaluation should begin if no pubertal development has occurred by age 13, if menarche has not occurred by age 15, or if menarche has not occurred within five years of thelarche. The differential diagnosis of primary amenorrhea encompasses that of secondary amenorrhea and includes pregnancy, hyperprolactinemia, thyroid dysfunction, hypothalamic-pituitary dysfunction, primary ovarian insufficiency related to chromosomal abnormalities, and polycystic ovarian syndrome. The differential diagnosis expands to congenital absence of the vagina, low transverse vaginal septum, imperforate hymen, and 46, XY disorders such as androgen insensitivity and 17α-hydroxylase deficiency when a blind vaginal pouch is encountered. A thorough history and physical examination should be the first step in the primary amenorrhea work-up [4].
Evaluation of a patient with primary amenorrhea should include a vaginal exam, uterine assessment, serum β-human chorionic gonadotropin, follicle-stimulating hormone, luteinizing hormone, prolactin, and thyroid-stimulating hormone levels. Karyotype analysis should be considered when differentiating testicular feminization and Turner syndrome (45, XO) from Mayer-Rokitansky-Küster-Hauser (MRKH) Syndrome. Free and total testosterone, as well as dehydroepiandrosterone sulfate, should be considered if signs of hyperandrogenism, such as virilization or hirsuitism, are present. Estradiol levels can be obtained if signs of estradiol exposure (eg. thelarche) are not present. Progesterone levels can be obtained, followed by a progesterone challenge test to confirm functional anatomy if a uterus is indeed present. Transvaginal ultrasound should be first choice in imaging to assess for müllerian anomalies. A magnetic resonance imaging of the abdomen and pelvis can then be used to further describe those findings seen on screening transvaginal ultrasound. Lastly, if ultrasound and MRI are not yielding, laparoscopy can be performed to assess for degree of MRKH anomalies [5].
While MRKH Syndrome physical examination reveals normal height, body hair distribution, secondary sexual characteristics, and external genitalia, the patient will often have an absent vagina or shortened blind pouch without a cervix. Careful evaluation of abdominal, urinary tract, and skeletal structures is recommended as up to 53% of MRKH syndrome patients will have congenital malformations.
MRKH Syndrome was described between 1829 by physiologist Mayer (1829), Rokitansky (1938), Küester (1910), and gynecologist Hauser (1961) [1] and is the second most common cause of primary amenorrhea, behind gonadal dysgenesis. MRHK syndrome has an incidence of 1 per 4000-10000 females and results from interrupted embryonic development of the paired müllerian (paramesonephric) ducts between the fourth and twelfth week of gestation. These ducts normally fuse distally into the lower two-thirds of the vagina and uterus, but remain independent proximally to form the fallopian tubes. In 2% to 7% of patients with MRKH syndrome, active endometrial tissue can be identified. Ovarian development is normal given the separate embryologic source. The molecular basis for MRKH syndrome has yet to be identified but multiple genes are being investigated. Genetic transmission is believed be in an autosomal dominant fashion with incomplete penetrance and variable expressivity [2,5].
There are three forms of MRKH Syndrome: typical, atypical, and MURCS (Müllerian duct aplasia, renal aplasia, cervico-thoracic somite dysplasia). These classes are further differentiated based on uterine anomaly using the American Fertility Society classifications (A and B). The typical form represents 47% of MRKH syndrome patients and is defined as development of fallopian tubes, ovaries, and renal system. The atypical form represents 21% of MRKH syndrome patients and is defined as malformations of the ovary or renal systems. MURCS represents 32% of MRKH syndrome and is associated with skeletal and/or heart malformations, muscular weakness, and renal malformations. The renal system seems to be most affected in MRKH syndrome due to the early interaction of the müllerian (paramesonephric) and wolffian (mesonephric) ducts [3].
A comprehensive approach to the management of MRKH syndrome patients is necessary and should include psychosocial counseling (healthy sexual practices, emotional stability, and fertility options such as assisted reproductive techniques and use of a surrogate). Vaginal reconstructive techniques to include progressive vaginal dilators and surgical techniques to produce a neovagina (e.g. Abbe-McIndoe operation or Veccheietti procedure) should be considered. Progressive vaginal dilation produces a functional vagina in 90-95% of patients and should be attempted prior to any surgical approaches [2].
A thorough history and physical exam, is critical in the evaluation of primary amenorrhea in the primary care setting. In this case, Mayer-Rokitansky-Küster-Hauser Syndrome was diagnosed. A multidisciplinary and comprehensive approach must be sought for these patients. Early involvement with specialty care is necessary to discuss nonsurgical and surgical options as well as provide psychosocial support.
-
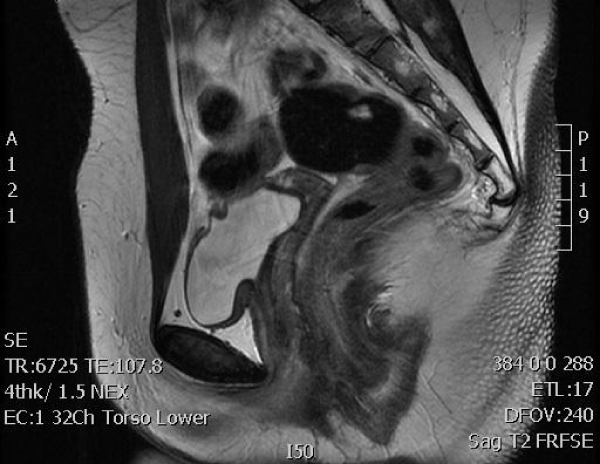
Figure 2:
Magnetic Resonance Imaging of the pelvic structures without evidence of uterine tissue.
-
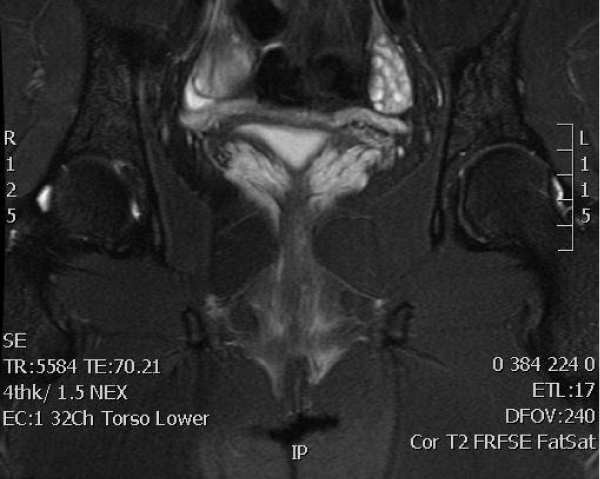
Figure 5:
Magnetic resonance imaging showing bilateral ovarian development without uterine structures.
Consent
Written informed consent was obtained from the patient's legal guardian for publication of this case report and any accompanying images.
Conflicts of Interest
We do not have any relevant financial relationships with any commercial entity. The information expressed above do not reflect the official policy of the Department of the Army, Department of Defense, or the U.S. Government.
Authors' Contributions
BB completed the literature review, informed consent, primary authorship of this article, and submission. RC was aided in an independent literature review, editing, and authorship of this article. DN was the overseeing attending provider who provided structural, grammatical, and clinical oversight. The authors acknowledge Dr. Cristóbal S. Berry-Cabán who contributed substantial editions to this paper.
- Committee on Adolescent Health Care (2013) Committee opinion: no. 562: müllerian agenesis: diagnosis, management, and treatment. Obstet Gynecol 121: 1134-1137.
- Oppelt P, Renner SP, Kellermann A, Brucker S, Hauser GA, et al. (2006) Clinical aspects of Mayer-Rokitansky-Kuester-Hauser syndrome: recommendations for clinical diagnosis and staging. Hum Reprod 21: 792-797.
- Folch M, Pigem I, Konje JC (2000) Müllerian agenesis: etiology, diagnosis, and management. Obstet Gynecol Surv 55: 644-649.
- Klein DA, Poth MA (2013) Amenorrhea: an approach to diagnosis and management. Am Fam Physician 87: 781-788.
- Pizzo A, Laganà AS, Sturlese E, Retto G, Retto A, et al. (2013) Mayer-rokitansky-kuster-hauser syndrome: embryology, genetics and clinical and surgical treatment. ISRN Obstet Gynecol 2013: 628717.




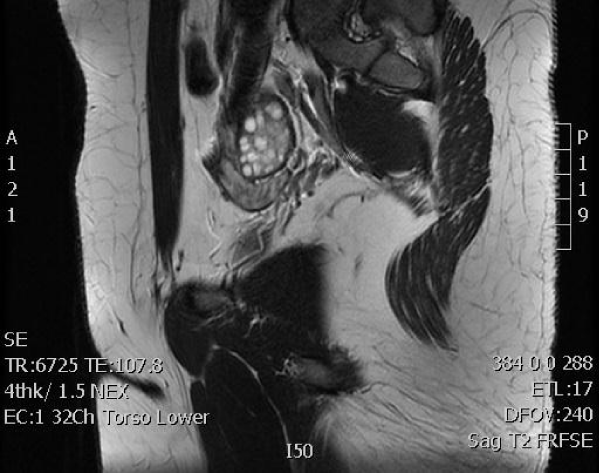
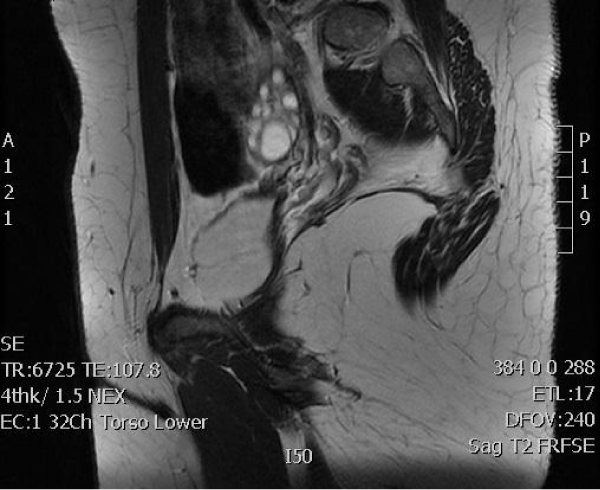





Figure 1:
Exploratory laparatomoy revealed bilateral ovarian development, bilateral fallopian tubes, and no uterine structures. An excision of a cyst was performed and confirmed by tissue review to be a paraovarian cyst rather than a uterine horn reminant. Notable structures in this photo include ovaries, fallopian tubes, and colon. No pelvic exam was done at this exam by the general surgeon.
Figure 1: Exploratory laparatomoy revealed bilateral ovarian development, bilateral fallopian tubes, and no uterine structures. An excision of a cyst was performed and confirmed by tissue review to be a paraovarian cyst rather than a uterine horn reminant. Notable structures in this photo include ovaries, fallopian tubes, and colon. No pelvic exam was done at this exam by the general surgeon.