Authors:
Rama Kumari Badyal, Jasmina Ahluwalia* and Kim Vaiphei
Departments of Histopathology and Hematology*, Postgraduate Institute of Medical Sciences and Research, Chandigarh, India
Received: 01 August, 2017; Accepted: 01 September, 2017; Published: 04 September, 2017
Kim Vaiphei, Professor, Department of Histopathology, Anand Block, Postgraduate Institute of Medical Sciences and Research, Chandigarh, India, Pin – 160012, Tel: +91 9815912943; Fax: 0172 2744401; E-mail:
Rama Kumari B, Ahluwalia J, Vaiphei K (2017) Myointimal hyperplasia of mesenteric vein- an experience in a tertiary care centre. Arch Clin Gastroenterol 3(3): 074-079. 10.17352/2455-2283.000044
© 2017 Rama Kumari B, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Myointimal hyperplasia; Mesenteric veins; Intestinal ischemia; Inflammatory bowel disease; Colitis; Tuberculosis; ymphoma
IMHMV: Idiopathic Myointimal Hyperplasia Of Mesenteric Vein; IBD: Inflammatory Bowel Disease; MIVOD: Mesenteric Inflammatory Veno-Occlusive Disorder; EVG: Elastica Van Giesen; MT: Masson’s Trichrome; IHC: Immunohistochemistry; SMA: Smooth Muscle Actin; PT: Prothrombin Time; APTT: Activated Partial Thromboplastin Time; PC: Protein C; PS: Protein S; ATIII: Anti-Thrombin III; FVL: Factor V Leiden Mutation; ACA: Anti-Cardiolipin Antibody; CECT: Contrast Enhanced Computed Tomography; IPSID: Immunoproliferative Small Intestinal Disease
Background: Idiopathic myointimal hyperplasia of mesenteric vein (IMHMV) is an extremely rare cause of venous mesenteric ischemia. It is defined as non-thrombotic occlusion of the mesenteric veins secondary to myointimal hyperplasia. IMHMV is a poorly understood condition involving the rectosigmoid colon predominantly young previously healthy male individuals
Purpose - to analyze surgically resected bowel specimens reported routinely as intestinal ischemia for the presence of features of IMHMV. There were 30 IMHMV of 118 cases that had been reported as intestinal ischemia.
Results: Clinical and laboratory findings in these 30 cases were re-evaluated. Mean age was 41.83±21.67 years and male female ratio was 5:1. Common presenting symptoms were abdominal pain (93.3%), diarrhoea (70%) and rectal bleeding (40%). Left colon was commonest site of involvement followed by right colon and ileum. Unique histological features observed were variable grades of fibrosis with subserosal and submucosal small to medium size veins showing myointimal proliferation. Thirteen of these 30 patients had associated intestinal stress conditions like strictures, torsions, volvulus and intussusceptions. Majority of these patients were investigated further for hypercoagulable states and were documented to be negative.
Conclusion: IMHMV is a selflimited condition where surgical resection of the affected segment is sufficient for a definitive treatment and needs to be recognized to avoid further unwarranted “management”.
Background
Idiopathic myointimal hyperplasia of mesenteric vein (IMHMV) is a rare disease described by Genta and Haggitt in 1991 [1]. It is a poorly understood disease frequently involving rectosigmoid usually in healthy young males. Often it is mistaken for inflammatory bowel disease (IBD) or mesenteric inflammatory veno-occlusive disorder (MIVOD) [2]. IMHMV usually presents with rectal bleeding or bloody stool resembling IBD. The diagnosis is established at histopathological examination of the surgical resected specimen in which the veins show intimal smooth muscle proliferation with normal accompanying arteries. IMHMV has been described mainly in the territory of inferior mesenteric venous drainage [3]. It has a benign clinical course and does not relapse after surgical resection of the affected intestinal segment [4]. Incidence of IMHMV is not known, likely to be under recognized and is important to differentiate from other conditions like IBD and intestinal tuberculosis. The present study was undertaken to determine prevalence of IMHMV in a tertiary care centre in surgical resected specimens retrospectively in cases that had been reported as ischemic enterocolitis, and to evaluate clinical profiles and laboratory parameters.
Material and Methods
We retrospectively evaluated cases that had been routinely reported as intestinal ischemia, by examining the hematoxylin and eosin (H&E) stained slides. We studied the major veins and arteries and the smaller sub-mucosal vessels. We also evaluated the clinical profiles and the laboratory parameters form the patient records. There were 118 cases which had been reported as ischemic enterocolitis over five years i.e. from 2011 to 2016. Site wise distributions of these 118 cases included left (34 cases) and right (48 cases) segmental colonic resections, total colectomy (10 cases), segmental resections of small bowel (20 cases), and resection of colostomy site (6 cases).
In the present study the term pre-resection trauma refers to the bowel segment that had been exposed to significant mechanical pressure and stress like volvulus, intussusceptions, obstruction due to stricture (inflammatory and/or neoplastic) and revision surgery. Clinical diagnoses included subacute and acute intestinal obstruction, bowel gangrene, gastrointestinal bleed, IBD, bowel perforation, volvulus, intussusceptions, diverticulitis, malignant stricture and stomal take down (Tables 1,2). A particular section was selected and the same was subjected further to histochemistry stainings like elastica Van Giesen (EVG), Masson’s trichrome (MT) and immunohistochemistry (IHC) for smooth muscle actin [SMA; clone 1A4, Dako, Denmark; dilution 1:100]. Blood vessels present at different bowel segment and layers of bowel wall were evaluated for myointimal smooth muscle hyperplasia, thrombosis, inflammation and necrosis. Of the 118 cases evaluated, 30 showed myointimal hyperplasia in varying sized veins at varying layer in the bowel wall. Clinicopathological features of these 30 cases were evaluated and all were subjected to further investigation for prothrombotic state which included prothrombin time (PT), activated partial thromboplastin time (APTT), protein C (PC) and S (PS), anti-thrombin III (ATIII), Factor V Leiden mutation (FVL), anti-cardiolipin antibody (ACA) and anti-ẞ2GP1 testing (B2GPI). Pro-thrombotic work-ups were carried out after a minimum gap of six weeks following the surgical procedure and four weeks after completion of oral anticoagulation therapy.
-

Table 2:
IMHMV cases in patients with history of mechanical stress or trauma.
Statistic evaluation
Frequencies of myointimal hyperplasia observed in veins were evaluated with respect to previous history of pre-resection trauma in different clinical conditions and were compared using Pearson Chi-square test. All calculations were performed using SPSS® version 17 (Statistical Packages for the Social Sciences, Chicago, IL).
Results
Thirty (25%) of 118 cases showed histological features of myointimal hyperplasia of the mesenteric veins (MIHMV) in minor and major branches. Distributions of the involved segments in these 30 resected specimens were - nine left colon, six right colon, five total colectomy, nine small bowel, and one colonic stomal takedown. Nineteen (63%) patients were between 10 to 50 years, and 11 (37%) were between 50 to 90 years, mean age = 41.83±21.67. There were 25 males and 5 females (M:F=5:1). Table 3 shows demographic, clinical and laboratory parameters and histopathological features. Presenting symptoms in these 30 patients were abdominal pain in 28 (93.3%), diarrhea in 21 (70%), lower gastrointestinal bleeding in 12 (40%), constipation in nine (30%) and abdominal distension in eight (26.6%). Two were known patients of diabetes mellitus and one patient of essential hypertension.
-

Table 3:
Clinical, and laboratory parameters in 30 patients with MIHMV.
Pre-resection colonoscopy in 20 patients revealed - i) diffuse mucosal ulceration involving left colon in 12 patients with rectal sparing and ii) multiple pseudopolyps and short segment strictures in sigmoid colon in eight. Contrast enhanced computed tomography scan (CECT) of abdomen available in 11/30 patients showed large bowel segmental mural thickening in six (20%) and thickened jejunal loops in two patients (6%). Three (10%) of them showed thrombosis of the portal and superior mesenteric veins (Figure 1) along with thrombosis of the superior mesenteric artery in two (6.6%). One more patient had presented with sub-acute intestinal obstruction. He was found to have jejunal stricture on endoscopy and the biopsy of which showed features of advanced stage of immunoproliferative small intestinal disease (IPSID). He was put on CHOP regimen. After one year of completion of CHOP regimen, he presented with fresh complaints of abdominal distension, diarrhoea and pedal oedema. Abdominal CECT showed pneumoperitoneum with evidence of sealed perforation and thickened small bowel loops. He deteriorated progressively and sustained cardiac arrest and died. At autopsy proximal jejunum showed two cm long stricture with serosal fibrosis and adhesion. Sections from this site showed extensive transmural fibrosis with mild degree of chronic inflammatory cell infiltration. There was no residual tumor. Sub-serosal and sub-mucosal veins were grossly occluded by myointimal and fibrointimal proliferations. There was another case who was clinically diagnosed as Tubercular stricture of ileo-caecal region. Histopathology of the resected specimen showed features of MIH in sub-serosal and sub-mucosal veins with no evidence of Tuberculosis. Tables 1 and 2 highlighted case distributions in different clinical conditions.
-
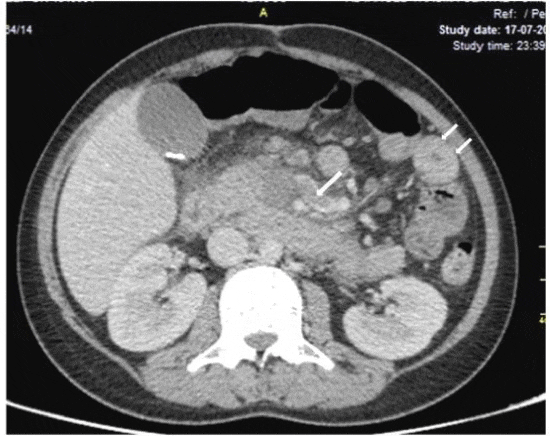
Figure 1:
Computerized tomography axial image (venous phase) showing hypodense filling defect in a tributary of superior mesenteric vein (arrow) and thickened jejunal loops (short arrows) in left upper abdomen.
Out of 118 examined, 20 cases were associated with history of pre-resection mechanical stress or trauma (Table 2) - Tubercular stricture (8), volvulus (2), intussusceptions (3), incarcerated hernia (5), revision surgery for IBD and stomal take down procedures (2) for Hirschprung’s disease. Among these 20 cases, only 13 (65%) showed features of IMHMV. The remaining 98 cases were diagnosed as perforations/gangrene (30), IBD (22), lower GI bleed (23), superior mesenteric vein thrombosis (8), colonic diverticular disease (8), Meckel’s diverticulum (5) and enteric duplication cysts (4). Seventeen (17%) of these 98 patients showed features of IMHMV on histology Pearson Chi-square test showed statistically significant association between IMHMV-like changes and history of pre-resection mechanical stress or trauma (p<0.001; Odds ratio of 8.849).
Histopathological features of the involved segment in 30 cases. All cases showed deep mucosal ulcers, granulation tissue formation and variable degree of lamina propria and submucosal fibrosis. Veins located in submucosa and subserosa were standing out as they appeared larger as the result of extensive thickening of the vessel wall by the proliferating myointimal cells with narrowing of the lumen and adventitial fibrosis (Figures 2A,B). There were two cases that had shown organized thrombi in the accompanying arteries and one case showed necrotizing vasculitis (Figure 2C) with no evidence of systemic vasculitis clinically. EVG staining confirmed the vessels with classic features to be veins (Figures 2D,E) and the proliferating cells to be smooth muscles by SMA immunostaining (Figure 2F). Majority of the cases (86.6%) showed transmural acute and chronic inflammatory cell infiltration with submucosal fibrosis and fat infiltration, and subserosal fibrosis. Mesenteric fat showed fat necrosis with collections of foamy histiocytes and fibrosis. In none of the cases, the adjoining colonic mucosa did not show features to suggest either chronic or active colitis, thereby a diagnosis of associated active IBD could be excluded. None of the cases showed any features both in gross and histology features that might suggest toxic megacolon (Figure s3A,B).
-
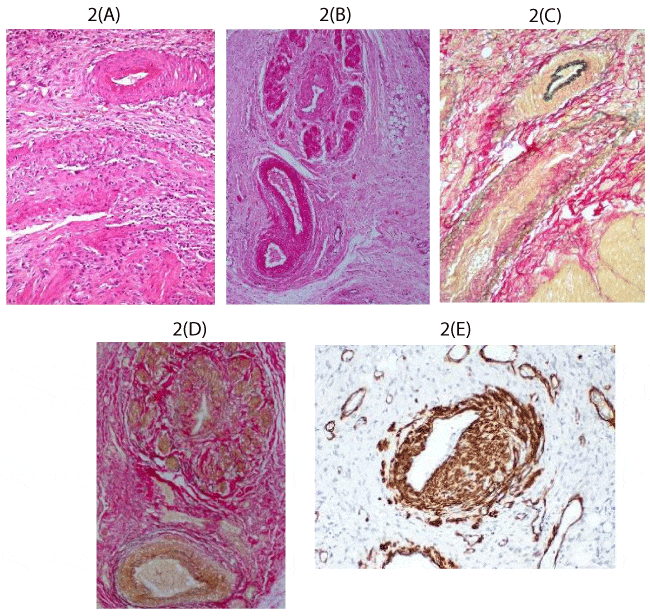
Figure 2:
A and B - Medium power photomicrographs to show occluded veins by myointimal proliferation and marked adventitial fibrosis. The accompanying arteries are relatively of normal morphology (H&E, x20). C and D - medium power photomicrograph of the same area to confirm the venous nature of the occluded vessels in Elastic Van Giesen stained sections (EVG, x20). E - medium power photomicrograph to show the proliferating cells occluding the vascular lumen to be of smooth muscle cell (Peroxidase anti-peroxidase, x20).
-
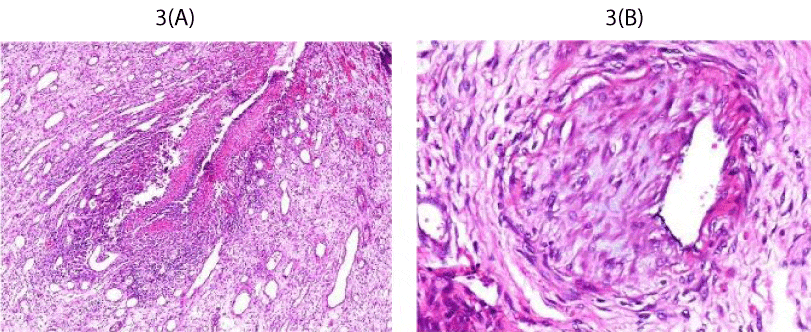
Figure 3:
A- medium power photomicrograph of a vein to show necrotising inflammation of the vessel wall (H&E, x20). B- medium power photomicrograph of a vein to show near total occlusion of the lumen by a recanalized thrombus (H&E, x20).
Treatment and follow up: All 30 patients underwent segmental resections of the involved bowel segments. Follow up is available in 20 of the 30 patients including the two patients with thrombosis of the accompanying arteries and all patients were doing well 12 to 40 months after post-surgery. Two patients died of unrelated causes and autopsy was done in one patient which had been highlighted in the result section. Table 4 describes the clinicopathological features of the reported series. Pro-coagulant work up could be carried out in 12(40%) patients during the follow-up period for PT, APTT and Fbrinogen which were within normal limits. All the 12 patients were negative for factor V Leiden, protein C and S, Lupus anticoagulant, Anti-thrombin III, Anti-cardiolipin antibody and Beta 2 glycoprotein I antibody.
-

Table 4:
Comparison of different studies of myointimal hyperplasia of mesenteric veins.
Discussion
Mesenteric ischemia usually occurs in elderly individual due to arterial thromboembolism [5]. Venous thrombosis causing ischemia is uncommon and accounts only for 5 to15% in reported series [6-10]. Non-thrombotic occlusion of mesenteric vein is a rare occurrence and have been associated with systemic lupus erythematosus, Behçet’s disease and mesenteric inflammatory veno-occlusive disease (MIVOD) [7-10]. IMHMV is an extremely rare etiology for venous mesenteric ischemia and is defined as a non-thrombotic occlusion of mesenteric vein due to myointimal hyperplasia [4]. Till date, about 26 IMHMV cases have been reported in the English literature [1-4,11-20]. In the literature, age ranged from 20 to 81 years (median of 45.2±16.08 years) and 72% being ≤50 years. In our study, age ranged between 5 to 85 years (mean of 41.83±21.67 years) and majority (63.3%) were ≤50 years of age. And the sex ratio in our study is similar to the reported series [4,11,15,17]. The common presenting symptoms in our cases were abdominal pain, diarrhoea and rectal bleeding, similar to the reported symptoms [7,13-15,17,19]. In the reported series, rectosigmoid region has been cited as the commonest site of involvement [4,11,14,16], which is similar to the present study. Dominant involvement of rectosigmoid region by IMHMV has led to the speculation of the underlying etiology to be related to an increased mobility of this bowel segment resulting in repeated vascular trauma resulting in myointimal hyperplasia in the involved relatively hypoxic veins [2,21-23].
Underlying etiology of IMHMV still remains obscure. Abu-Alfa et al. [2], hypothesized segmental arteriovenous fistulization secondary to torsion or stretching injury to be the underlying etiology for myointimal hyperplasia (MH) in the affected veins, as in sigmoid mesocolon which is far more mobile than other colonic segment. This hypothesis has been supported by Sherman et al. [4]. In the present study, 13 (65%) of the 30 patients with history of bowel trauma or pressure, though the remaining 17 patients did not have any such existing history. There was highly significant association with trauma and presence of MHMV (p<0.001), with the Odds ratio of 8.849. Hence, our study also supports the theory of pre-resection trauma to be likely underlying etiological factor for MH. In a single case report where intake of nonsteroidal anti-inflammatory drug for chronic back pain had been blamed for the development of MHMV [13]. Bryant [11], also reported similar pathology in a 42-year- old hypertensive woman who died of sudden cardiac death and he attributed the changes in mesenteric vein to long standing propranolol intake. In our series, there was one patient who was on antihypertensive agents and two diabetic patients. Diabetes per se is also known to result in proliferation of smooth muscle cells occluding vascular lumina due to associated hypoxia.
IMHMV has also been seen in association with factor V Leiden mutation and the morphological changes observed in the veins were thought to be the result of increased high pressure perfusion of venous collaterals after thrombosis of major mesenteric vein. Hence, IMHMV may be considered in the clinical differential in patients with history of deep venous thrombosis or familial thrombophilia presenting with IBD like clinical symptoms, who fails to show characteristic mucosal changes and do not respond to medical therapy for IBD [14]. In the present study fibrin thrombi were observed in the affected veins in 10 patients. However, the pro-coagulant tests were negative. Flaherty et al. [6], suggested IMHMV to be a late stage of MIVOD or enterocolic lymphocytic phlebitis, as seven of their patients who had intestinal ischemia, three showed evidence of MHMV along with active phlebitis and venulitis. They had used the termed MIVOD by hypothesizing that it might be a precursor lesion of MHMV. Small bowel IMHMV had also been reported in association with appendiceal mucocoele and pseudomyxoma peritonei [16]. We also have one patient who was treated for IPSID and had developed MH one year after completion of chemotherapy. Most reported cases of IMHMV were considered clinically to be IBD and were invariably treated with steroids and other specific anti-inflammatory drugs which might result in reduction of inflammation [17,24-26]. Potential overlap between the two disorders is highlighted in a reported case as enterocolic lymphocytic phlebitis or mesenteric inflammatory veno-occlusive disorder [25]. In all documented cases of IMHMV, the diagnoses had been established on histological examination of the surgical resection specimens as the diagnostic features were not obvious in mucosal biopsies and in none of these reports and our cases did not have any associated mucosal changes of IBD [17,18]. Recently reported findings of subtle angiographic changes may have a supportive role in the diagnosis of IMHMV [26].
Conclusion
IMHMV is a rare condition observed commonly amongst young males. The present study highlights importance of subjecting resected specimens to routine pathological examinations, difficulties of recognizing this entity only on clinical, radiological and endoscopic features. Surgical resection of the affected bowel segment is the only curative treatment. There was no abnormal coagulation parameter in our patients. Awareness amongst the pathologists as well as clinicians especially surgeons, will help to identify this group of patients, with a possible idiopathic etiology thereby preventing administration of unwarranted chemotherapeutic agent.
Acknowledgements
We express our gratitude to all the staffs of the department histopathology for helping us to complete the study.
-
-
-
- Genta RM, Haggitt RC (1991) Idiopathic myointimal hyperplasia of mesenteric veins. Gastroenterology 101: 533-539. Link: https://goo.gl/42x9uX
- Abu-Alfa AK, Ayer U, West AB (1996) Mucosal biopsy findings and venous abnormalities in idiopathic myointimal hyperplasia of the mesenteric veins. Am J Surg Pathol 20: 1271-1278. Link: https://goo.gl/sn2afs
- Blaszyk H, West AB (2005) Idiopathic myointimal hyperplasia of the mesenteric veins: a rare diagnostic pitfall. Am J Gastroenterol 100: 1423-1424. Link: https://goo.gl/kuHxXa
- Shermana J, Kaob PC, Westc AB, Blaszyka H (2006) Focal myointimal hyperplasia of mesenteric veins is associated with previous trauma in surgical specimens. Pathol Practice Research 202: 517-522. Link: https://goo.gl/kxtVy4
- Wangensteen KJ, Fogt F, Kann BR, Osterman MT (2015) Idiopathic myointimal hyperplasia of the mesenteric veins diagnosed preoperatively. J Clin Gastroenterol 49: 491–494. Link: https://goo.gl/bxRbMf
- Flaherty MJ, Lie JT, Haggitt RC (1994) Mesenteric inflammatory veno-occlusive disease: a seldom recognized cause of intestinal ischemia. Am J Surg Pathol 18: 779-784. Link: https://goo.gl/KeUjsu
- Saraga E, Bouzourenne H (2000) Enterocolic (lymphocytic) phlebitis: a rare cause on intestinal ischemic necrosis. A series of six patients and a review of the literature. Am J Surg Pathol 24: 824-829. Link: https://goo.gl/ZMwEaF
- Hu JC, Forshaw MJ, Thebe P, Stewart M (2005) Mesenteric inflammatory venoocclusive disease as a cause of acute abdomen: report of five cases. Surg Today 35: 961-964. Link: https://goo.gl/svxeFK
- Ngo N, Chang F (2007) Enterocolis lymphocytic phlebitis: clinicopathologic features and review of the literature. Arch Pathol Lab Med 131: 1130-1134. Link: https://goo.gl/Mg2YdF
- Costa MN, Saiote J, Pinheiro MJ, Duarte P, Bentes T, et al. (2016) Segmental colitis caused by idiopathic myointimal hyperplasia of mesenteric veins. Rev Esp Enferm Dig 108: 821-826. Link: https://goo.gl/9GU2zc
- Bryant J (1998) Unexpected sudden death during propranolol therapy in a patient with mild mesenteric venous myointimal hyperplasia. J Forensic Sci 43: 905-907. Link: https://goo.gl/3McMYZ
- Savoie LM, Abrams AV (1999) Refractory proctosigmoiditis caused by myointimal hyperplasia of mesenteric veins: report of a case. Dis Colon Rectum 42: 1093-1096. Link: https://goo.gl/iQvpxE
- Kao PC, Vecchio JA, Hyman NH, West AB, Blaszyk H (2005) Idiopathic myointimal hyperplasia of mesenteric veins: a rare mimic of idiopathic inflammatory bowel disease. J Clin Gastroenterol 39: 704-708. Link: https://goo.gl/rKwjWY
- De Hertogh G, Van Eyken P, Stessens L, Caenepeel P, Geoboes K (2005) Myointimal hyperplasia of mesenteric veins secondary to heterozygous factor V Leiden mutation. Histopathol 47: 322-334. Link: https://goo.gl/ECv1ga
- García-Castellanos R, Lopez R, de Vega VM , Ojanguren I, Pinol M, et al. (2011) Idiopathic myointimal hyperplasia of mesenteric veins and pneumatosis intestinalis: A previously unreported association. J Crohns Colitis 5: 239-244. Link: https://goo.gl/EUKtai
- Lanitis S, Kontovounisios C, Karaliotas C (2012) An extremely rare small bowel lesion associated with refractory ascites. Idiopathic myointimal hyperplasia of mesenteric veins of the small bowel associated with appendiceal mucocoele and pseudomyxoma peritonei. Gastroenterology 142: e5-e7. Link: https://goo.gl/3oid1W
- Korenblit J, Burkart A, Frankel R, Klinge M, Greenbaum L, et al. (2012) Refractory pancolitis: a novel presentation of idiopathic myointimal hyperplasia of mesenteric veins. Gastroenterol Hepatol (NY) 8: 696-700. Link: https://goo.gl/ifNsnK
- Feo L, Cheeyandira A, Schaffzin DM (2013) Idiopathic myointimal hyperplasia of mesenteric veins in the elderly. Int J Colorectal Dis 28: 433-434. Link: https://goo.gl/ryg8uu
- Chiang CK, Lee CL, Huang CS, Huang SH, Wu CH (2012) A rare cause of ischemic proctosigmoiditis: idiopathic myointimal hyperplasia of mesenteric veins. Endoscopy 44: E54-E55. Link: https://goo.gl/arPvMp
- Thomas BS (2013) Myointimal hyperplasia of the mesenteric veins mimicking infectious colitis. Int J Colorectal Dis 28: 727. Link: https://goo.gl/4mGSBs
- Kern WH, Wells WJ, Meyer BW (1981) The pathology of surgically excised aortocoronary saphenous vein bypass grafts. Am J Surg Pathol 5: 491-496. Link: https://goo.gl/9xe779
- Chang KM (2007) New histologic findings in idiopathic mesenteric phlebosclerosis: clues to its pathogenesis and etiology-probably ingested toxic agent-related. J Chin Med Assoc 70: 227-235. Link: https://goo.gl/ymFk3n
- Platz J, Hyman N (2012) Idiopathic Myointimal Hyperplasia of Mesenteric Veins. Gastroenterol Hepatol (NY) 8: 700-702. Link: https://goo.gl/8q8svA
- Gan SI, Urbanski S, Coderre SP, Panaccione R (2004) Isolated visceral small artery fibromuscular hyperplasia-induced ischemic colitis mimicking inflammatory bowel disease. Am J Gastroenterol 99: 2058-2062. Link: https://goo.gl/9pXMSe
- Lavu K, Minocha A (2003) Mesenteric inflammatory veno-occlusive disorder: a rare entity mimicking inflammatory bowel disorder. Gastroenterology 125: 236-239. Link: https://goo.gl/g86JGh
- Jevon GP, Ravikumara M (2010) Endoscopic and histologic findings in pediatric inflammatory bowel disease. Gastroenterol Hepatol 6: 174-180. Link: https://goo.gl/nFnqNj









Table 1:
IMHMV cases in patients with no history of mechanical stress or trauma.
Total number of cases available for histological examination of resected specimens
----------------------------------------------------------------------
IBD (18)
Subacute or acute intestinal obstruction (13)
Colonic diverticular disease (8)
Enteric duplication cysts (4)
Lower GI bleeding (18)
Small and large intestinal erforations/gangrene (24)
Mesenteric venous thrombosis (8)
Meckel’s diverticulum (5)
Number of cases (%) with
IMHMW
--------------------------------------------
2
7
1
0
2
3
2
0
Total (98)
17
IMHMV -Idiopathic myointimal hyperplasia of mesenteric veins.