Author(s):
Kai-Yuan Hsiao1, Chiang-Shin Liu2, Tung-Yiu Wong1,3, Jehn-Shyun Huang1,3, Ken-Chung Chen1,3 and Tze-Ta Huang1,3*
1Division of Oral and Maxillofacial Surgery, Department of Stomatology, National Cheng-Kung University Medical College and Hospital, Tainan, Taiwan
2Department of Pathology, National Cheng-Kung University Medical College and Hospital, Tainan, Taiwan
3Institute of Oral Medicine, National Cheng-Kung University Medical College and Hospital, Tainan, Taiwan
Received: 27 February, 2015; Accepted: 19 March, 2015; Published: 21 March, 2015
Tze-Ta Huang, Division of Oral and Maxillofacial Surgery, Department of Stomatology, Institute of Oral Medicine, National Cheng-Kung University Medical College and Hospital, Tainan, Taiwan, Tel: 886-6-2353535-2964; Fax: 886-6-2359885; Email:
Hsiao KY, Liu CS, Wong TY, Huang JS, Chen KC, Huang TT (2015) Oral Mucosa Malignant Melanoma: Clinical Features, Diagnosis, Treatment, and a Case Report. J Dent Probl Solut 2(2): 019-024. DOI: 10.17352/2394-8418.000011
© 2015 Hsiao KY, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Oral mucosal malignant melanoma; Adjuvant radiotherapy; Immunohistochemical markers; Palatal mucosa
CK: Cytokeratin; LCA: Leukocyte Common Antigen; PET: Positron Emission Tomography; MRI: Magnetic Resonance Imaging; MITF: Microphthalmia Transcription Factor; FASN: Fatty Acid Synthase
Primary oral mucosa malignant melanoma is a rare and biologically aggressive neoplasm. It is estimated about 1~2% of all oral malignancies with the incidence increasing with age. The prognosis of oral mucosa malignant melanoma is poor with the five-year survival rate is approximately 15%. The diagnosis of oral melanoma is usually delayed because it is always asymptomatic at the beginning and it resembles the epulis, amalgam tattoo or other oral lesions. In addition, nearly a third of all oral melanoma are amelanotic and may lack a radial growth phase, which makes early and accurate diagnosis even difficult. Thus, regional and distant metastases happen more frequently. Surgery is the first choice of treatment, and clinically negative necklymph nodes with neck dissection or radiotherapy are also recommended because of the high risk of subclinical regional metastasis.
In this article, we reviewed the clinical features, diagnosis, treatment, and presented a 70 y/o male who suffered from an easily bleeding lesion over right posterior palatal mucosa and gingiva who presented at hospital for help. We performed biopsy which revealed a malignant melanoma. He received supraomohyoid neck lymph node dissection, partial maxillectomy, and was reconstructed with anterior lateral thigh free fascia cutaneous flap. After surgical treatment, the patient kept regular follow-ups. The treatment outcome was good and the patient recovered with full swallowing and phonation function.
Introduction
Melanoma is a malignant neoplasm of melanocytic origin that arises from melanocytes. Although most melanomas occur on skin, they may develop at any site where melanocytes are present. Approximately 91.2% of melanomas occur on skin surfaces, 5.2% on eyes and only 1% of melanomas arising from mucosal surfaces [1,2]. In the mucosal surfaces, about 55.4% are presented in head and neck region. These make primary oral mucosa malignant melanoma extremely rare. In the oral cavity, the most common primary sites are hard palate and maxillary mucosa. Buccal mucosa, mouth floor, mandibular gingiva are rare affected sites. The etiology of oral mucosa malignant melanoma is still unknown. No apparent relationship of oral mucosa constantly exposing to chemical, thermal, or physical events was present [2].
Atypical melanocytes are initially seen at the epithelial and connective tissue junction. They are usually larger than normal melanocytes and have varying degrees of nuclear pleomorphism and hyperchromatism. In oral lesions, invasion of lymphatic and blood vessels are seen more readily than skin lesions [3]. Several mucosal melanomas have been reported to contain bone and cartilage like components. In some cases, they may have no melanin production (amelanotic melanoma). This may also be one of the challenges to make an accurate diagnosis because melanoma can mimic a variety of undifferentiated tumors. Histological differential diagnoses included malignant lymphoma, amelanotic melanoma, spindle cell malignancies of mesenchymal tissues, and undifferentiated carcinoma. Immunohistochemical studies such as S-100 protein, HMB-45, Melan-A and Mart-1 reactivity of the tumor cells are beneficial in distinguishing such melanomas from other malignancies [4].
The prognosis of oral mucosa malignant melanoma is extremely poor in relationship to its cutaneous counterpart. The 5-year survival rate is around 13%~22%. It may be resulted from delayed diagnosis and treatment, the aggressive nature of the disease, difficulty in achieving wide resection and a tendency for early hematogenous metastasis. Therapy of oral mucosa malignant melanoma is commonly based on surgical excision of the primary tumor, but it may be challenge depending on the anatomic location within the oral cavity and extent of tumor. Although melanoma is traditionally considered to be radioresistant, some authors have described improved survival and local control with postoperative radiotherapy [1,4]. In some studies, chemotherapy and immunotherapy are served as adjunctive therapies. However, there are still no guidelines or consensus in treatment of oral mucosa malignant melanoma. In this article, we reported a case of primary oral mucosa malignant melanoma over right maxillary gingiva and palatal mucosa. The clinical features, histopathological and image findings, treatments and post-operative follow up are presented.
Case
A 70-year-old male was referred to our department due to a painless but easily bleeding mass over right upper posterior gingiva. The patient was without any systemic disease also denied alcohol consumption, betel nut chewing or smoking habit. He had suffered from the above episode for 4 months and did not seek medical treatment because it was relatively small and initially asymptomatic. However, the swelling mass grew larger and started to bleed afterwards. Then he went to dental clinic for help and was referred to Department of Oral and Maxillofacial Surgery, National Cheng Kung University Hospital, Taiwan.
During oral examination, there was an ulcerative red-purple lesion measuring 3.0 x 2.0 cm in size with bleeding tendency over right posterior palatal gingiva. An incisional biopsy was suggested and performed at the same visit. Pathological section reveals a malignant melanoma, characterized by proliferative epithelioid cells with marked cytological atypia, frequent mitoses (more than 15 per 10 high power field), and dense lymphoid aggregation. Junctional activity (Figure 1A) and focal melanin deposition (Figure 1B) are seen also.
Further immunohistochemical studies, the tumor cells revealed a positive S-100 (Figure 1C) and HMB-45 (Figure 1D). While CK (cytokeratin), LCA (leukocyte common antigen) and CD34 were negative.
From the imaging studies, the initial panoramic film (Figure 2) showed multiple missing posterior teeth, and the computed tomography scan revealed right maxillary sinusitis (Figure 3A,3B), with an enlarged lymph node over right neck level Ib (Figure 3C). Although no obvious bony destruction was noted from these examinations, increased radioactivity in right maxilla was shown in the whole body bone scan (Figure 4). According to these clinical characteristics, surgical intervention of malignant tumor ablative surgeries were suggested and accepted by the patient.
-
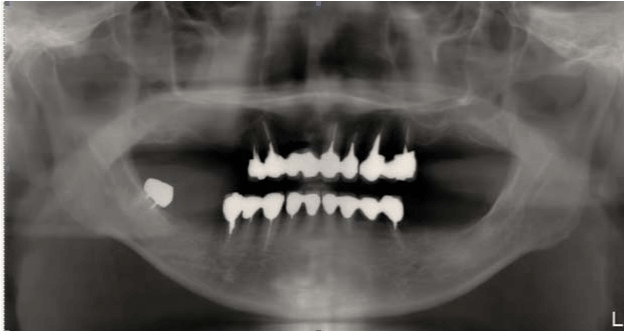
Figure 2:
The initial panoramic film showed multiple posterior teeth loss and full mouth prosthesis. The border of right upper alveolar bone showed a smooth surface and a homogenous radiopacity. No obvious bony destruction was found.
-
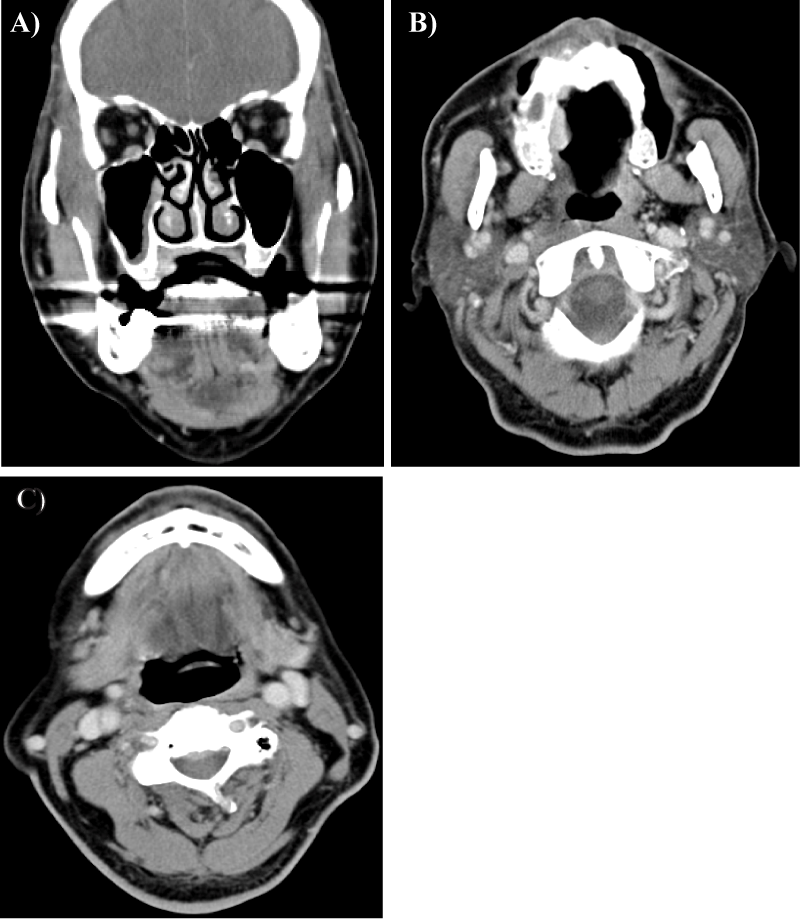
Figure 3:
(A, B) Computed tomography scan illustrated a smooth and intact border of right palatine bone. No bony invasion was indicated. Right maxillary sinusitis can also be found. (C) A enlarged lymph node (arrow) was noted at level Ib.
-
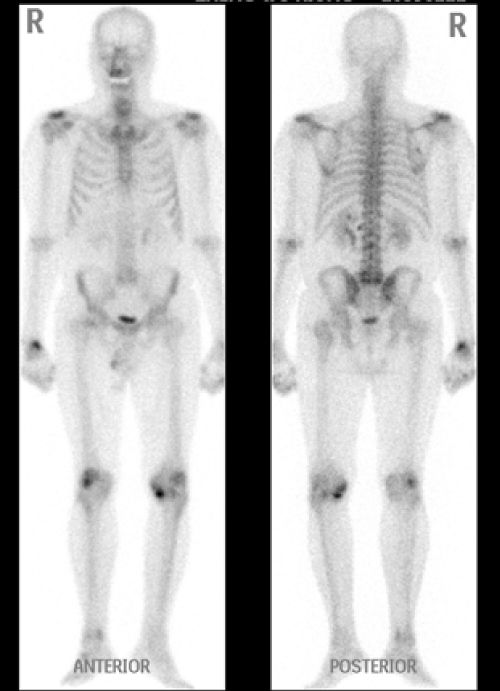
Figure 4:
Whole body bone scan showed increased radioactivity in right maxilla. No distant bony metastasis was favored.
Right neck lymph node dissection from level III to I was done. While neck lymph node dissection, frozen pathological section examination of neck lymph nodes in closest proximity to the tumor clinically were dissected out and revealed no evidence of metastasis. The tumor was widely excised combined with partial maxillectomy with 1.5cm safe margin (Figure 5A,5B). The frozen pathological section examination of surgical margins also revealed no evidence of tumor. The surgical defect was then reconstructed by left anterolateral thigh free fascia cutaneous flap (Figure 6). The patient tolerated the procedures smoothly and his general condition was well controlled. However, the color of free flap turned dark-red three days after the surgery. An emergency operation was performed to check the venous anastomosis. The venous return of anastomosis was compressed by blood clots and submandibular gland. After the blood clots were debrided and the submandibular gland was repositioned, the venous congestion of anterolateral thigh free fascia cutaneous flap improved. The flap was also de-epithelialized at distal edgeand dripped with heparin continuously for 6 days. The flap color turned pink and the ecchymosis gradually subsided.
-
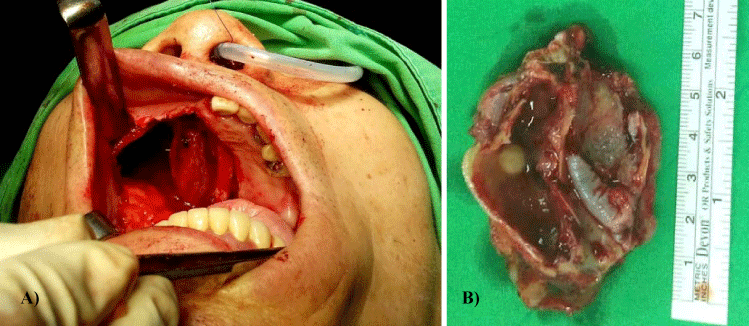
Figure 5:
(A) Tumor wide excision with a 1.5cm safe margin. The superiormargin was close to infraorbital rim; medial margin across the midline of palate; the posterior margin was close to pharyngeal and lateral pterygoidplate. (B) The vertical view of resected specimen. A nasal polyp was noted in the sinus (arrrow).
Postoperative histopathological examination confirmed the diagnosis of oral mucosa malignant melanoma. The tumor invaded into the submucosa layer, without evidence of maxillary invasion. Perineural tumor invasion was also present (Figure 7) however lymphovascular tumor emboli were not seen. All margins were free from tumor invasion (tumor away from resection margins: at least 7mm), and dissected lymph nodes were all free of tumor metastasis. Positron emission tomography (PET) and CT was done one month after the surgery, which showed some lymph nodes with increased Fludeoxyglucose (18F) (FDG) uptake in the right retropharyngeal and right neck level II areas (Figure 8A,8B). With these findings, the oncologist suggested close observation, and no adjunctive treatment was recommended. The appearance of the reconstruction flap (Figure 9) was well and there was no evidence of recurrence 6 months after the surgery. The patient was under periodical follow-up in oncology and our department.
-
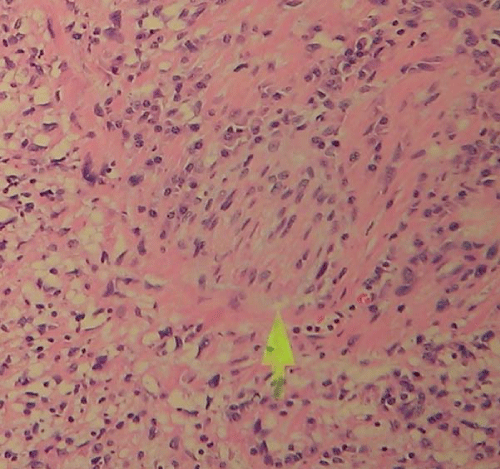
Figure 7:
The tumor cells were presented in nerve bundle (arrow), which suggested perineural invasion.
-
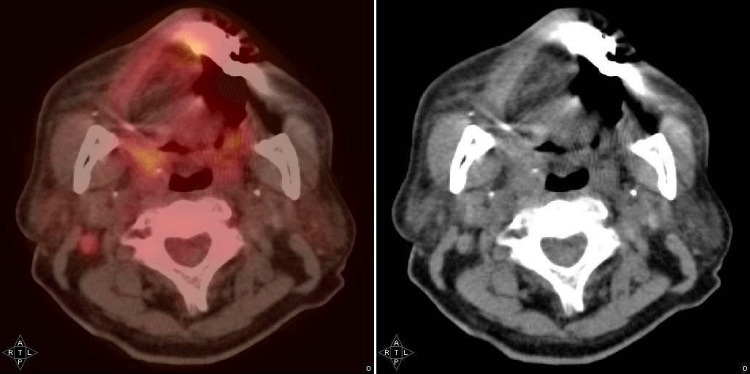
Figure 8:
Post-operation one month positron emission tomography and computed tomography scan. There are lymph nodes with increased FDG uptake in the right retropharyngeal and right neck level II areas.
Discussion
The oral mucosa malignant melanoma is a rare and invasive neoplasm. In contrary to cutaneous melanomas, the risk factors and pathogenesis are unclear and the prognosis is still poor. The most frequently affected oral sites are the palate and the maxillary gingiva. These oral sites accounting for about 77% of all oral mucosa malignant melanoma. The other affected sites are lower gingiva, buccal mucosa and mouth floor [5,6]. The age of patients range from 20 to 80 years, with the peak incidence from 41 to 70 years of age. There is a slight male predilection and more common in Japanese and African cultures [7]. In this report, the patient was a 70-year-old male and the tumor was located over right palatal mucosa and maxillary gingiva, which was consistent with the previous literature.
The clinical symptoms included swelling, bleeding, ill-fitting dentures, pain, tooth mobility and delayed healing of post extraction wounds. However, these are usually inconspicuous and could be easily ignored, making the diagnosis delayed and the tumor stage more advanced [8]. Regional lymphadenopathy may be present and connotes a poor prognosis [9]. The lesion is usually asymmetric with irregular borders, and the surface may be smooth or ulcerated. A variety of colors may show in oral malignant melanoma with black, brown, gray, purple and red. Sometimes it will be amelanotic which makes it particularly difficult to be diagnosed [2]. Furthermore, patients with non pigmented lesions appear to have a particularly poor prognosis [10]. In our patient, a red-purple, smooth surfaced painless mass was noted with bleeding tendency.
According to Greene et al. the diagnosis of oral mucosa malignant melanoma should involve three criteria: (1) demonstration of malignant melanoma in the oral mucosa; (2) present of junctional activity in the oral mucosa and (3) inability to show any other primary site [11]. However, melanoma metastasis may also involve the epithelial junction, however the presence of junctional activity is not reliable to indicate the lesion as a primary one. Dermoscopy may be utilized as an adjunctive tool in clinical differential diagnosis of oral mucosal melanoma, which allows easy differentiation of amalgam tattoos, “in situ” and invasive melanoma [3]. A flow-chart for the diagnosis of pigmented lesions in the oral mucosa and perioral tissues was suggested by Meleti et al. [12], which could excludes or includes melanoma by the following questions and examination step by step: medical history, melanotic or non-melanotic lesions, ABCD checklist, recent history, age and subsite. It may be a clear diagnostic sequence for general dentists to avoid unnecessary biopsy in some cases. If there is any uncertainty or the diagnosis cannot be made on clinical ground alone, tissue biopsy remains the definite procedure to confirm the final diagnosis.
In general, oral mucosa malignant melanoma can be diagnosed with the Hematoxylin and Eosin Stain. However, if there is only scarce melanin present or even none in amelanotic melanoma, immunohistochemical stains should be performed for further information. S100 is an acidic calcium binding protein, which is a very sensitive marker for cells derived from neural crest, such as Schwann cells, dendritic cells, nevi and melanoma cells. It has a high sensitivity but a limited specificity. HMB-45 is quite selective for melanogenic proteins gp100, which has a high specificity but a low sensitivity. Microphthalmia transcription factor (MITF), on the other hand, may have a better diagnostic value. It is the only nuclear melanocytic marker and appears to be both highly sensitive and highly specific histopathological melanocyte marker for melanoma [13,14]. To distinguish oral melanoma from melanocytic nevi, fatty acid synthase (FASN)can be a helpful marker [15]. CK and LCA stains are used for differential diagnosis of squamous cell carcinoma and lymphomarespectively. In our case, enough evidences were provided from the clinical and pathological findings to make the final diagnosis of oral mucosa malignant melanoma.
In imagingstudies, CT, Magnetic resonance imaging (MRI) and PET are all effective tools for evaluating primary lesion, local and distant metastasis. PET may be suitable for the staging or restaging of the mucosal malignant melanomain the head and neck [16]. In our patient, no local or distant metastasis was showed from the CT and PET scan.
Although there is still no guideline or consensus for the treatment of oral malignant melanoma, surgical intervention remains the treatment of choice. Umeda et al. suggested a surgical protocol:(1) primary lesion should be excised with a 15mm safe margin by an intraoral approach, (2) metastatic lymph nodes should be excised, (3)adjuvant immunochemotherapy should be considered [17]. Whether the prophylactic neck lymph dissection should be done is still controversial. Wuet al. suggested that the patients with cN0 nodular melanomas should have prophylactic neck lymph node dissection, while close observation is recommended for patients with cN0 macular melanomas. The patients with metastaticcervical lymph nodes should undergo radical neck resection [18]. On the contrary, Tanaka et al. [19] supported the viewpoint of Blatchford et al. [20] and Kristian et al. [21], that radical neck dissection should be reserved for confirmed lymph node metastasis and not done prophylactically, despite the propensity for melanoma to metastasize [17].
Additionally, postoperative radiotherapy is recommended if poor prognostic pathologic features are present. Meleti et al. reported the recurrence rate was lower in cases who undergo surgery with postoperative radiotherapy than surgery alone [2]. However, the post-operative radiotherapy did not improve the survival rate or decrease the distant metastasis rate. Prophylactic neck dissection was performed from level III to level I was performed on our patient with staging of pT3N0M0, stage III. The post operation pathological finding showed no lymph nodes or distant metastasis. However, perineural invasion was noted. The oncologists recommended close observation and no disease progression for 6 months to date.
Chemotherapy is considered for the metastatic melanoma or as a palliative treatment. Dacarbazine, interleukin-2, high-dose IL-2 and IFN-α are the drugs commonly used. However, these drugs do not seem to increase the survival rate of patients [22].
Recently, the breakthrough of targeted and immunotherapies in cancer treatment may lead an evolution for cancer treatment including melanoma due to its significant improvement in response and survival rates. Combination therapies of both targeted and immunotherapies for melanoma patients may further enhance the effectiveness and efficiency in cancer treatment. Up to date, Immunotherapies are only considered in cases with distant metastasis or when the primary tumor is not possible to be resected clearly [22]. Another novel treatment was conducted by the use of oncolytic virus. An attractive oncolytic virus known as “T-VEC (talimogene laherparepvec)” was reported as a safe and potentially effective antitumor therapy in treating malignant melanoma in a randomized controlled Phase III study by Hughes et al. [23]. The positive outcomes in treating malignant melanoma with these new concepts bring us new strategies to combat the oral mucosa malignant melanoma. However, there are still some issues to be addressed as which patient responds to these drugs. What are the strategies to schedule or combine these drugs to achieve the best outcome and cause the least side effects? Therefore, there are definite benefits to further studies that identify pathogenesis and outcome analysis of the oral mucosa malignant melanoma.Conclusion
Oral mucosa malignant melanoma is an aggressive tumor with rapid progression and tendency for hematogenous metastasis. It is also extremely difficult to identify early signs and to diagnose at an early stage. Achieving an adequate wide excision is the gold standard to treatment. However, it is very challenging to achieve when the intraoral tumor grows very large. The prognosis could be improved by careful oral mucosa inspection, early diagnoses, proper and prompt treatment. Further improvement of prognosis of oral mucosa malignant melanoma requires more sufficient pathogenesis studies and outcome analysis of this rare disease. Our patient was treated with neck lymph node dissection, wide excision of the tumor with 1.5cm safe margin combined partial maxillectomy and reconstructed with anterior lateral thigh free fascia cutaneous flap. The treatment protocol followed the suggestions of the published literatures. There is no disease progression for 6 months. Longer follow up is needed to assess our treatment protocol.
Acknowledgement
Special thanks for contribution to the medical staff of 7B ward, Operative Room, Department of Anesthesiology, BICU, and Department of Stomatology, National Cheng Kung University Hospital, Taiwan, R.O.C. for caring the patient.
- Stanley F Malamed (2014). Hand book of local anesthesia. Elesiver6th edition 96.
- Daniel M Laskin. Oral and maxillofacial surgery. Mosby 2nd edition page 41.
- Larry J Peterson. Contemporary oral and maxillofacial surgery. Mosby 4th edition page 45.




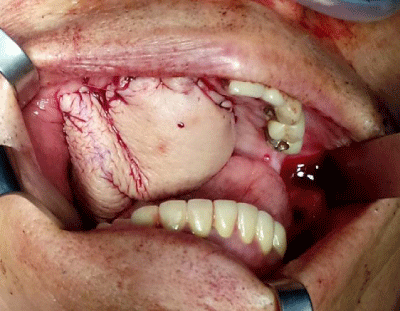
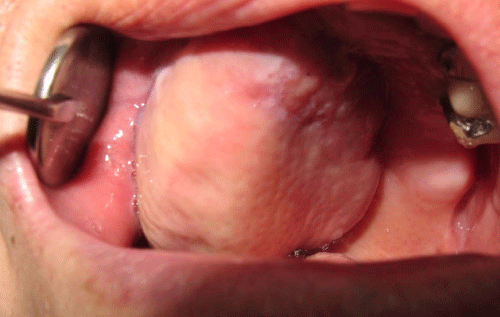





Figure 1:
(A) H&E stain showed hyperchromatin, polymorphic neoplastic cells with cytological atypia. Abundant mitotic figures was also presented. These suggest a malignant appearance. (B) Melanin (arrow) was noted near the border of incised lesion. (C) S-100 stain was positive and showed high sensitivity. (D) HMB45 stain was positive. The sensitivity seemed lower than S-100 stain.
Figure 1: (A) H&E stain showed hyperchromatin, polymorphic neoplastic cells with cytological atypia. Abundant mitotic figures was also presented. These suggest a malignant appearance. (B) Melanin (arrow) was noted near the border of incised lesion. (C) S-100 stain was positive and showed high sensitivity. (D) HMB45 stain was positive. The sensitivity seemed lower than S-100 stain.