Author(s):
Marianne Terrasse1,2, Florence Jouan2, Thibault Dolley-Hitze1,2, Yannick Arlot-Bonnemains2, Marc-Antoine Belaud-Rotureau2,3, Nathalie Rioux-Leclercq2,4, Nolwenn Lorcy1,2and Cécile Vigneau1,2
1CHU Pontchaillou, Service de Néphrologie, 2 rue Henri Le Guilloux 35033 Rennes Cedex, France
2Université Rennes 1, CNRS UMR6290, KyCa, 2 avenue du Professeur Léon Bernard, CS, 34317, 35043 Rennes Cedex, France
3CHU Pontchaillou, Service de cytogénétique, 2 rue Henri Le Guilloux 35033 Rennes Cedex, France
4CHU Pontchaillou, Service d'anatomie et cytologie pathologiques, 2 rue Henri Le Guilloux 35033 Rennes Cedex, France
Received: 14 July, 2015;Accepted: 26 October, 2015; Published: 28 October, 2015
Dr. Marianne Terrasse, Université Rennes 1, CNRS UMR6290, KyCa, 2 avenue du Professeur Léon Bernard, CS, Tel: 0033 2 99 28 43 96; Tel: 0033 2 99 28 43 96; Fax: 0033 2 99 28 41 50; Fax: 0033 2 99 28 41 50; E-mail:
Terrasse M, Jouan F, Dolley-Hitze T, Arlot-Bonnemains Y, Belaud-Rotureau MA, et al. (2015) Anti-VEGF Therapy Induces Proteinuria through Endothelial Disorganization Leading to Nephrin Decrease in Podocytes. Int J Immunother Cancer Res 1(1): 021-028.10.17352/2455-8591.000006
© 2015 Terrasse M et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Glomerular slit diaphragm; Targeted anti-VEGF therapy; Sunitinib; Podocytes; Actin cytoskeleton
Background: VEGF is involved in cancer development by stimulating neo-angiogenesis and tumor proliferation. Anti-angiogenic therapies, especially tyrosine kinase inhibitors such as sunitinib, have significantly improved cancer prognosis. Nevertheless, renal side effects, such as proteinuria and thrombotic microangiopathy, have been reported. The underlying physiopathological mechanisms remain unclear, but animal models and clinical similarities with preeclampsia suggest that such therapies affect the function of the endothelial and epithelial layers of the glomerular basement membrane, with activation of the endothelin signaling system and loss of glomerular slit diaphragm integrity. The aim of this in vitro study was to determine sunitinib effects on normal podocytes and glomerular endothelial cells.
Methods: The glomerular microvascular endothelial (GMVEC) and human glomerular visceral epithelial (hGVE) cell lines were incubated with various doses of sunitinib. The MTT Cell Proliferation Assay was used to assess cell proliferation. Expression of nephrin (a major slit diaphragm protein) and endothelin was evaluated by immunofluorescence or western blotting assays.
Results: Sunitinib inhibited GMVEC and hGVE cell proliferation in a dose-dependent manner. In GMVEC cells, endothelin transcription and secretion were increased after incubation with sunitinib. Conversely, in hGVE cells, sunitinib did not affect nephrin expression. However, conditioned medium from GMVEC cells incubated with sunitinib modified nephrin expression when added to the culture medium of hVGE cells. This effect was inhibited by pre-incubating hGVE cells with an endothelin inhibitor.
Conclusion: This study suggests an indirect toxicity of sunitinib on podocytes through endothelin. Therefore, sunitinib-induced renal side effects could be controlled with endothelin inhibitors.
Introduction
Vascular endothelial growth factor (VEGF) plays a key role in tumor angiogenesis and in metastasis spreading. In the last decade, anti-angiogenic therapies targeting the VEGF pathway have revolutionized the treatment of metastatic cancer [1]. They include the anti VEGF monoclonal humanized antibody bevacizumab and tyrosine kinase inhibitors, such as sunitinib, that target especially VEGF receptors (VEGF-R) [2]. Such therapies have significantly improved progression-free survival and overall survival [3-5]. Therefore, sunitinib is now recommended as first-line therapy for patients with metastatic renal cell carcinoma, breast cancer and gastrointestinal stromal tumors [6].
However, anti-VEGF drugs can induce several adverse effects (gastrointestinal disorders, skin toxicity and hypertension) that may require dose reduction or discontinuation in half of the patients. Proteinuria after treatment with bevacizumab is observed in 21% to 63% of patients [7], but renal adverse effects may have been underestimated. Indeed, diagnostic kidney biopsies, which are rarely performed in these patients, have highlighted some cases of immuno-allergic interstitial nephritis [8], focal segmental glomerulosclerosis [9], acute tubular necrosis [10], and more frequently thrombotic microangiopathy (TMA). These lesions are potentially reversible after drug discontinuation [11-14]. Recently, we included 22 patients in the RARe database (Registry of patients with major kidney side effects during treatment with anti-VEGF drugs) [15]. Analysis of the renal biopsies from these patients indicated the presence of acute or chronic TMA in 21. Specifically, the observed lesions (glomerular endothelial cell swelling, loss of endothelial fenestrae and effacement of foot processes) were reminiscent of the alterations observed in preeclampsia [15]. Indeed, there are clinical and pathophysiological similarities between preeclampsia and the renal side effects of anti-VEGF treatments [21].
During preeclampsia, expression of the soluble form of VEGF-R1 (sFLT-1) increases, whereas VEGF serum level decreases [16]. By binding and neutralizing VEGF, sFLT1 inhibits the VEGF signaling pathway. This leads to disorganization of vascular endothelial (VE) cadherin a key component of endothelial cell-cell junctions [19], and consequently to increased vascular permeability and proteinuria. It has been reported that VEGF-A phosphorylates VEGF-R2 and VE-cadherin, ultimately resulting in disassembly of intercellular junctions and increased permeability of the glomerular slit diaphragm [20].
Moreover, histological analysis of kidney biopsies from patients with preeclampsia revealed the presence of TMA, with reduced formation of endothelial fenestrae. In mice, injection of sFLT-1 induces a “preeclampsia-like syndrome” with acute hypertension, edema, TMA histological lesions and reduction in nephrin expression [14]. In kidney biopsies from patients treated with anti-VEGF agents, VEGF, synaptopodin and nephrin expression levels are decreased [15], whereas the endothelin signaling system, which stimulates VEGF production [22], is activated [23,24]. Similarly, in preeclampsia, expression of nephrin and synaptopodin is reduced [25]. Loss of nephrin could be due to shedding from the cell surface through endothelin-1 release by endothelial glomerular cells [26].
These studies suggest that the proteinuria induced by anti-VEGF drugs is a consequence of the dysregulation of the slit diaphragm, leading to endothelial and epithelial cell dysfunction. Therefore, the aim of this study was to determine the in vitro effects of sunitinib on normal podocytes and glomerular endothelial cells. Cell-cell interactions in cells incubated with sunitinib were studied to test the hypothesis of endothelin-1 (ET-1) implication, as described in preeclampsia.
Materials and Methods
Cell lines and cell culture methods
The human glomerular visceral epithelial cell line hGVE (i.e., podocytes) was generously given by Pr. Rondeau (INSERM U702, Paris, France) [27]. Cells were cultured in Dulbecco's Modified Eagle Medium/Nutriment Mixture F-12 (DMEM/F-12; Gibco®, Carlsbad, USA) with 5% fetal bovine serum (FBS) (PAA Laboratories®, Pasching, Austria), 1% Penicillin- Streptomycin solution (10000 U/mL penicillin + 10000µg/mL streptomycin, Gibco®) and in extempo 1% of 100X Insulin-Transferrin-Selenium-X Supplement (Gibco®). Cells were cultured in 25cm³ or 75cm³ tissue culture flasks.
The commercial glomerular microvascular endothelial cell line (GMVEC) (ACBRI 128 – CellSystems®) was isolated from normal human renal cortex. Cells were cultured in EGM™2 SingleQuots® (Lonza® Walkersville, USA), containing 5% FBS, 0.04% hydrocortisone, 0.4% human fibroblast growth factor, 0.1% VEGF, 0.1% ascorbic acid, 0.1% human epidermal growth factor, 0.1% arginine 3 – insulin-like growth factor, and 0.1% GA-1000 solution (30 mg/ml gentamycin + 15 µg/ml amphotericin).
Sunitinib: kindly supplied by Pfizer® (New-York, USA), was dissolved in dimethylsulfoxide (DMSO) to a 10mM stock solution stored at -20°C. Supernatants of GMVEC cells incubated with sunitinib or DMSO (called conditioned medium) were used to treat hGVE cells. The endothelin receptor-A (ET-RA) antagonist BQ-123 (Sigma-Aldrich®, Saint-Louis, USA) was dissolved in sterile water to a 0.4mM or 400µM stock solution and stored at -20°C.
MTT Cell Proliferation Assay: To analyze cell proliferation, 2000 cells/well were plated in 96-well plates. Three days later, cells were incubated or not with sunitinib and proliferation was assessed after 24, 48 and 72 hours using the colorimetric MTT Cell Proliferation Assay (Sigma-Aldrich®, Saint-Louis, USA), according to the manufacturers protocol. Absorbance at 550nm was measured with a FLUO-star Omega spectrophotometer (BMG Labtech®, Offenbourg, Germany). Experiments were done in triplicate.
RNA purification
RNA was extracted using the RNeasy® Mini Kit according to the manufacturer's protocol (Qiagen®, Venlo, Netherlands). RNA concentration was determined in duplicate using a Nano Drop ND-1000® spectrophotometer (Thermo Scientific®, Wilmington, USA).
Quantitative polymerase chain reaction (qPCR)
Reverse transcription (RT): For each sample, 2µg of RNA were mixed with 7µL reaction mix and RNAse-free water to a final volume of 25µL. The reaction mix contained 5µL 5X reaction buffer (250mM Tris-HCl, 375mM KCl, 15mM MgCl2, 50mM DTT) (Promega® M531A), 0.5µL of 10mM dNTP mix (Promega® U151B), 1µL of 500μg/ml Random Primers (Promega® C118A), 0.2µL of 40U/μL RNasin Plus RNase Inhibitor (Promega® N261A) and 0.3µL of 200U/μL M-MLV Reverse Transcriptase® (M170A, Promega®, Madison, USA). RT was performed in triplicate in a PTC 200-Peltier Thermal Cycler (MJ Research), according to the manufacturer's instructions. Complementary DNA samples were stored at -20°C.
Sequence-specific oligonucleotide primers: Primers were purchased from Eurogentec® (Seraing, Belgium) or Sigma®. GAPDH: forward, 5'-CTGACTTCAACAGCGACACC-3' and reverse, 5'-TAGCCAAATTCGTTGTCATACC-3'; ET-1: forward, 5'TCTCTGCTGTTTGTGGCTTG-3' and reverse, 5'-GAGCTCAGCGCCTAAGACTG-3'; VEcadherin: forward, 5'-ACCCCCACAGGAAAAGAATC-3' and reverse, 5'ACACACTTTGGGCTGGTAGG-3'; ET-RA: forward, 5'-GCGCTCTTAGTGTTGACAGGT3' and reverse, 5'-GAATCCCAATTCCCTGAACA-3'; synaptopodin (SYNPO): forward, 5'AGGGAGGACCTAGCAGACG-3' and reverse, 5'-GTCAGCTGGGCTGCAATC-3'.
Relative quantification by real-time PCR was performed using the Applied 7900HT Fast Real-Time PCR System (Applied Biosystems™) and the Power SYBR® Green PCR Master Mix (Applied Biosystems™, Foster City, USA). Experiments were done in triplicate. Double-distilled water blanks and samples reverse transcribed without reverse transcriptase served as negative controls for each run.
Western blot analysis
Protein extraction: Cells were rinsed twice with phosphate-buffered saline (PBS: 10mM sodium phosphate, pH 7.5, 0.9% saline), and then proteins were extracted with cold lysis buffer (20mM Tris-HCl pH 7.5 (Sigma Aldrich®, Saint-Louis, USA), 100mM NaCl, 5mM MgCl2, 0.5mM dithiothreitol, 20mM β-glycerophosphate, 0.2% Nonidet-P40, 10% glycerol, 10µL/mL Protease Inhibitor Cocktail Set IV® (Calbiochem®, Gibbstown, USA) and 200µL/mL Phosphatase Inhibitor Cocktail Set III® (Calbiochem®, Gibbstown, USA)). Extractions were performed at 4°C for 30min and by nitrogen freezing and heating to 37°C for 30min, and then samples were centrifuged at 13.000rpm for 30min.
Protein concentration: The protein concentration of each sample was determined with the Bradford Reagent B6916 (Sigma-Aldrich®) and bovine serum albumin (BSA) (Sigma®) as protein standard. Absorbance was determined by spectrophotometry on a Jenway 6051 Colorimeter (Jenway®, Felsted, UK).
Electrophoresis: Protein extracts (20µg of each sample) were diluted with 3X Laemmli Buffer (3% SDS, 15% β-mercaptoethanol, 30% glycerol, 0.03% BBP, 1.5M Tris HCl pH 7.5, 3mM EDTA) and denatured at 95°C for 5 min. They were then were separated on 10% SDSpolyacrylamide gels in 10% of 10X Tris-Glycine Buffer (BioRad®, Munich, Germany) and 0.1% SDS using a Power PAC 1000 BioRad® generator following the manufacturer's instructions. Protein Molecular Weight Marker Odyssey® was used as reference. Proteins were then transferred to polyvinylidene fluoride membranes (Thermo Scientific®) with transfer buffer (10X Tris-Glycine, BioRad®).
Immunodetection: Membranes were blocked in 5% dry milk/0.1% Tris-Buffered Saline (50mM Tris-HCl pH 7.4; 150mM NaCl)/0.05% Tween-20 (TBST) for 1hr and then with primary antibodies diluted in 5% dry milk/0.1% TBST at 4°C overnight. Table 1 lists the used primary antibodies. After several rinses with 5% dry milk/0.1% TBST, the appropriate peroxidase-conjugated secondary antibodies were added at room temperature for 1hr. Membranes were washed three times with 0.1% TBST and developed with SuperSignal®
West Dura Extended Duration Substrate (ThermoScientific™, Rockford, USA), using the Curix 60® apparatus (AGFA®, Mortsel, Belgium). Actin expression was tested as loading control. Signal intensity was quantified using the Imagequant™ TL software (GE Healthcare Bio-Sciences AB®, Uppsala, Sweden).
Immunofluorescence staining (IF)
Cells were grown on glass slides. GMVEC cells were fixed at 4°C with 95% ethanol for 30min, followed by acetone at room temperature. hGVE cells were fixed at -20°C with methanol for 3min. For VE-cadherin expression analysis, cells were permeabilized in 0.2% Triton X-100 in PBS for 3 minutes and blocked with 3% BSA IF buffer (PBS, 3% BSA, 0.1% Tween 20) for 1 hour followed by 15 minutes incubation with 1% BSA IF buffer (PBS, 1% BSA, 0.1% Tween 20). Cells were then incubated with primary antibodies against VEcadherin or nephrin at room temperature in a humidified chamber for 1h30. After washing with 1% BSA IF buffer, cells were incubated with Alexa-fluor® 555 donkey anti-mouse IgG (H+L) (1:1000, Molecular Probes, USA). For actin staining, cells were incubated with rhodamine phalloidin conjugated to the red-orange fluorescent dye tetramethylrhodamine (1:100) at room temperature shielded from the light for 1h30. Nuclei were counterstained with DAPI/Anti-fade solution (Q-Biogene, MP Biomedicals, USA) and cells analyzed with a fluorescence microscope (LEICA® DMRXA, Germany).
Enzyme-linked immunosorbent assay (ELISA)
The human ET-1 QuantiGlo ELISA kit (R&D Systems®, Abingdon, United Kingdom) was used according to the manufacture's specifications. ET-1 concentration in aliquots of supernatants from GMVEC cells incubated or not with sunitinib was measured in duplicate. Results were analyzed with the Ascent Software, Multiskan RC (Thermo LabSystems®, Cergy-Pontoise, France), at the wavelength of 450nm.
Immunocytochemistry
Cells were plated on eight-well Labtech® chamber slides (30,000 cells/well). The following day, treatment was initiated. At the end of the treatment, cells were rinsed with PBS and fixed in 3.65% formaldehyde (36.7% Formol, Sigma-Aldrich®). Cells were then incubated with 10% hydrogen peroxide for 5min, followed, if needed, by permeabilization by incubation in 0.1% Triton X-100 in PBS for 3min. Blocking was performed with 3% BSA/PBS for 1h, followed by rinses with 1% BSA/PBS for 10min. Cells were stained with primary antibodies diluted in PBS for 1h30. Commercially available kits were used for secondary antibodies (Dual Link System-HRP, Dako®). Antibody reactions were revealed with 3.3diaminobenzidine (DAKO®, Glostrup, Denmark), followed by counterstaining with 0.5X hematoxylin. Slides were mounted with Faramount Aqueous Mounting Medium (DAKO®) and stored at room temperature. Images were acquired with a Leica® DFC 295 microscope.
Statistical analysis
Results are representative of at least three independent experiments performed in triplicate, unless otherwise mentioned. Results are expressed as the mean ± standard deviation (SD). Statistical analysis of the data was performed using the Student's t-test for independent variables and the R software (Bell Laboratories, USA). Differences were considered significant when p<0.05.
Results
Sunitinib reduces proliferation of hGVE and GMVEC cells
To test the in vitro effects of sunitinib on glomerular epithelial and endothelial cells, hGVE and GMVEC cells were plated in 96-well plates (2000 cells/well) and incubated with different concentrations (0.15µM, 1.5µM, and 5µM) of sunitinib or vehicle alone (DMSO; control cells). Cell proliferation/viability was then assessed with the MTT Cell Proliferation Assay at 24h (D1), 48h (D2), 72h (D3) and 96h (D4) after addition of sunitinib. Compared with control cells, sunitinib reduced proliferation/viability of both hGVE and GMVEC cells in a dose-dependent manner (Figure 1). The 5µM concentration was too toxic, leading to a high rate of cell mortality (data not shown) and therefore was not used in the subsequent experiments.
-
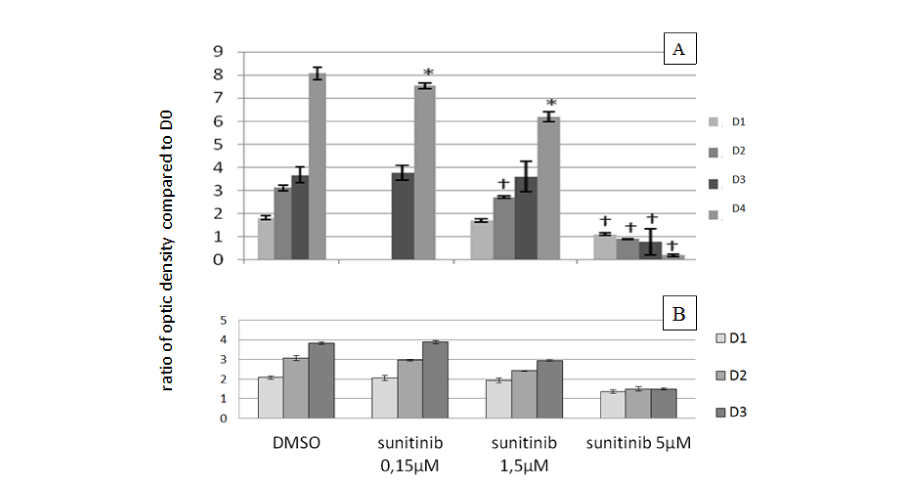
Figure 1:
Proliferation of sunitinib-treated hGVE (A) or sunitinib-treated GMVEC (B) by MTT proliferation assay. DMSO treatment (control) or sunitinib treatment begins at Day 0 (D0). Cellular growth is expressed every day as a ratio of optic density compared to D0 the same day. *: p<0.05 and †p<0.001 compared to DMSO control of the same day. Bars and intervals represent the mean ± standard deviation A. hGVE cells: sunitinib concentrations treatment: 0.15µM, 1.5µM or 5µM. For D4: 1 experiment. B. GMVEC cells: sunitinib concentrations treatment: 0.15µM, 1.5µM or 5µM.
Sunitinib does not affect slit diaphragm protein expression in hGVE cells
As nephrin expression is decreased in kidney biopsies from patients treated with anti-VEGF agents [15], we evaluated whether sunitinib directly affected nephrin expression in podocytes by western blot analysis of hGVE cells incubated with 0.15µM or 1.5µM sunitinib for 1 to 3 days. Sunitinib did not modify nephrin expression compared with untreated cells (DMSO) at any of the tested concentrations (Figure 2A). Similar results were obtained by immunocytochemistry analysis of hGVE cells incubated with 1.5µM sunitinib (b) or DMSO (a) for 48h (Figure 2B).
-
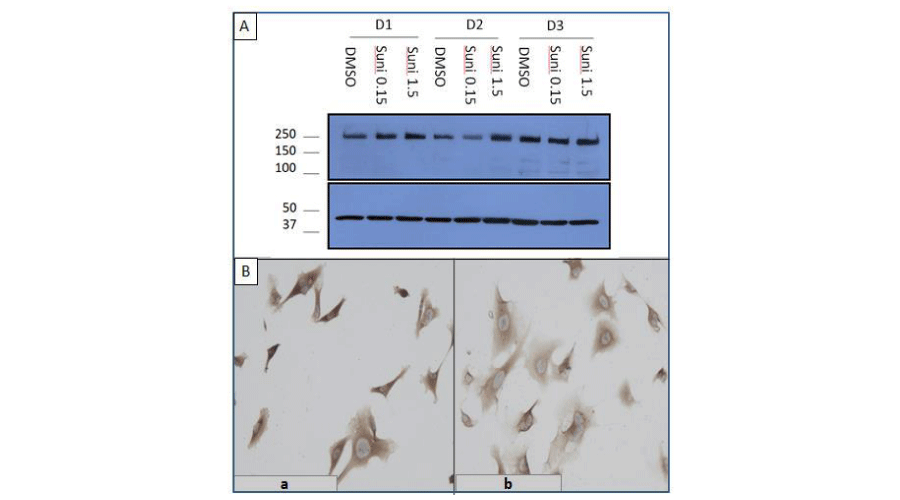
Figure 2:
Direct effect of sunitinib on nephrin expression by hGVE. A. by western-blotting. hGVE cells were incubated for 24h, 48h or 72h with sunitinib 0.15µM and 1.5µM. Control DMSO. Above: nephrin western-blot. Below: actin control. B. by immunocytochemistry. Representative micrographs of nephrin signaling detected by immunocytochemistry in hGVE cells incubated for 48h with DMSO (a), or with sunitinib 1.5µM (b). Original magnification x 40.
Sunitinib does not affect ET-1 and ET receptor type A expression in hGVE cells
As hGVE cells can synthesize ET-1, which regulates the VEGF pathway, and express endothelin receptor type A (ET-RA), we then evaluated whether sunitinib influenced their expression.
ET-RA expression was assessed by western blotting (Figure 3A) and RT-qPCR (Figure 3B) in hGVE cells incubated with sunitinib or DMSO for 24, 48 or 72h. A non-significant timedependent ET-RA increase was observed in DMSO- and sunitinib-treated cells (Figure 3A). ETRA protein and mRNA expression were not significantly different in DMSO- and sunitinib treated hGVE cells, although huge variations in expression were observed by RT-qPCR analysis.
-
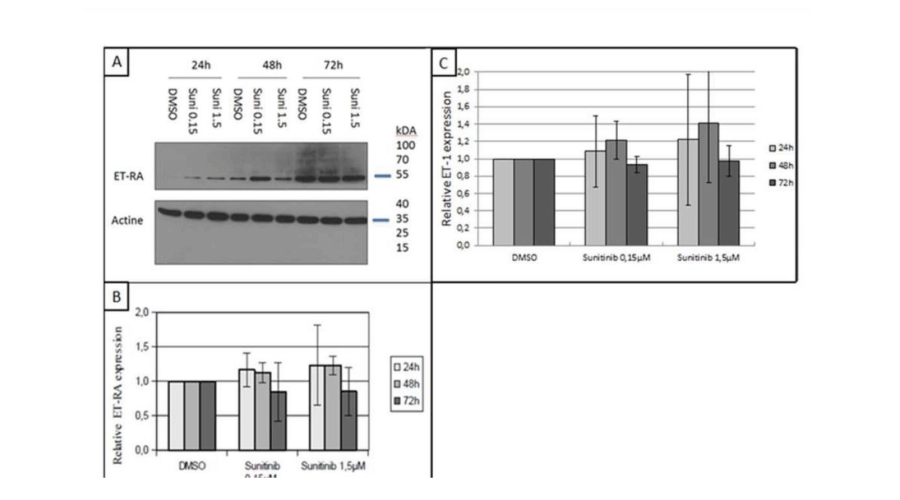
Figure 3:
Effects of sunitinib on endothelin receptor A (ET-RA) (A and B) and endothelin-1 (C) expression in hGVE cells. hGVE were incubated for 24h, 48h or 72h with sunitinib 0.15µM and 1.5µM. Control DMSO. A: analysis of Endothelin receptor A (ET-RA) expression evaluated by Western-blotting.
Similarly, RT-qPCR analysis of ET-1 expression in DMSO- and sunitinib-treated hGVE cells indicated that sunitinib did not affect its expression level (Figure 3C).
Sunitinib affects VE-cadherin organization and ET-1 expression in GMVEC cells
As in kidney biopsies from women with preeclampsia, cell-cell junctions are disturbed in activated glomerular endothelium and this endothelium secretes ET-1, we tested the effect of sunitinib also in GMVEC cells.
Immunofluorescence analysis of GMVEC cells incubated with sunitinib for 24 to 72 hours indicated that sunitinib treatment induced a disorganization of VE-cadherin localization (right panel) compared to DMSO-treated cells (left panel) (Figure 4a). This effect was not due to changes in VE-cadherin expression level because RT-qPCR quantification of VE-cadherin gene expression level indicated that it was not significantly different in treated and untreated cells, whatever the sunitinib concentration (Figure 4b).
-
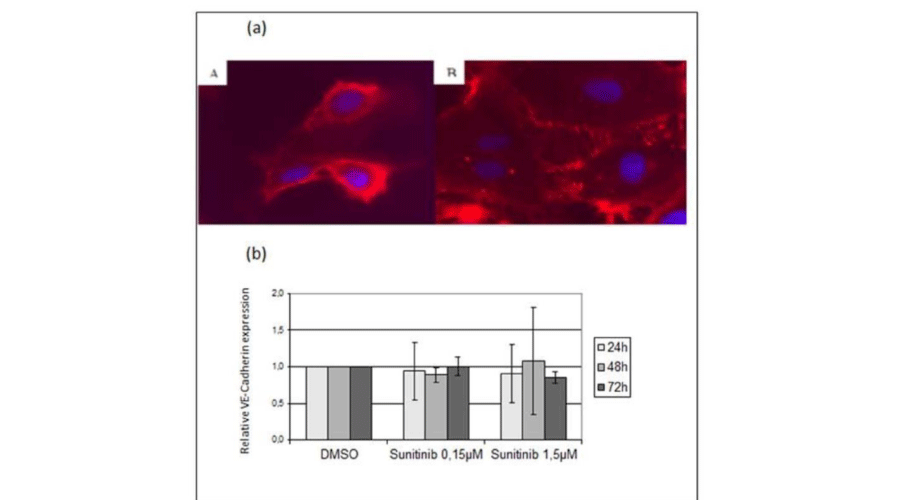
Figure 4:
Sunitinib action on GMVEC cell-cell interaction. GMVEC cells were treated by sunitinib 0.15µM or 1.5µM for 1 to 3 days. (a): disorganization of VE-Cadherin by immunofluorescence after 3 days of treatment by sunitinib 1.5µM (B) compared to DMSO (A). Original magnification x160. (b): VE-Cadherin gene expression by quantitative PCR. Control DMSO.
Conversely, incubation with 1.5 µM sunitinib induced an increase of ET-1 expression (Figure 5A) and probably secretion in GMVEC cells (Figure 5B) compared with DMSO-treated cells, although the difference was not significant due to the important result variability.
-
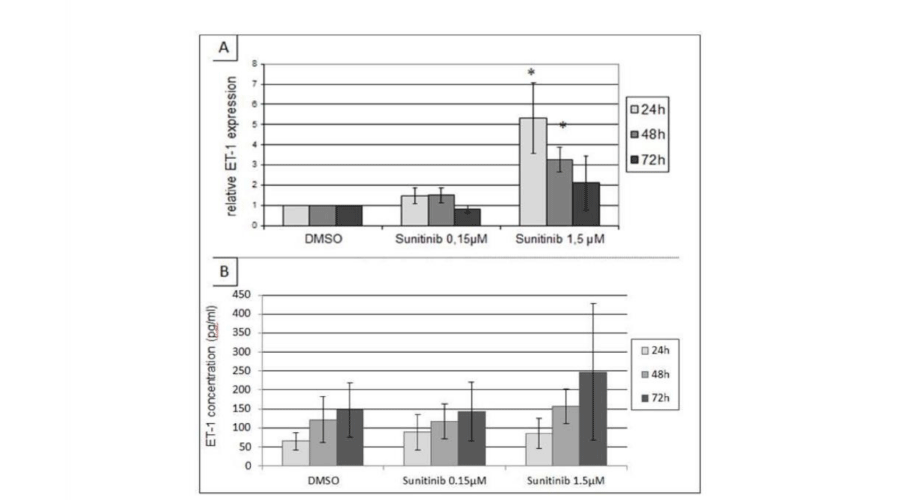
Figure 5:
Treatment by sunitinib increases ET-1 expression and secretion by GMVEC. A. ET-1 expression by quantitative PCR. GMVEC were treated for 1 to 3 days by sunitinib 0.15µM and 1.5µM. Control DMSO.*: p<0.05 compared to control DMSO. B. ET-1 secretion by GMVEC in the medium of culture by ELISA. Collection of supernatants of culture of GMVEC after 1, 2 or 3 days of treatment by sunitinib 0.15µM and 1.5µM. Control DMSO.
Conditioned medium from sunitinib-treated GMVEC cells affects nephrin expression and localization in hGVE cells
To try to understand the mechanism underlying nephrin expression reduction in kidney biopsies from patients treated with sunitinib, we hypothesized that sunitinib could alter indirectly the expression of slit diaphragm proteins through its effects on glomerular endothelial cells. To test this hypothesis, GMVEC cells were incubated with DMSO, 0.15µM or 1.5µM sunitinib and culture supernatant (called conditioned medium, CM) was collected after 24h, 48h and 72h. Then, hGVE cells were grown in the presence of the different CM (undiluted) and cell proliferation/viability and slit diaphragm protein expression were assessed.
Analysis of the results of the MTT proliferation assay indicated that cell proliferation/viability was not significantly different in hGVE cells grown in CM from GMVEC cells incubated with sunitinib (CM-Suni) or with DMSO (CM-DMSO) compared with cells grown in normal culture medium (DMEM), excepted after 72h (Figure 6).
-
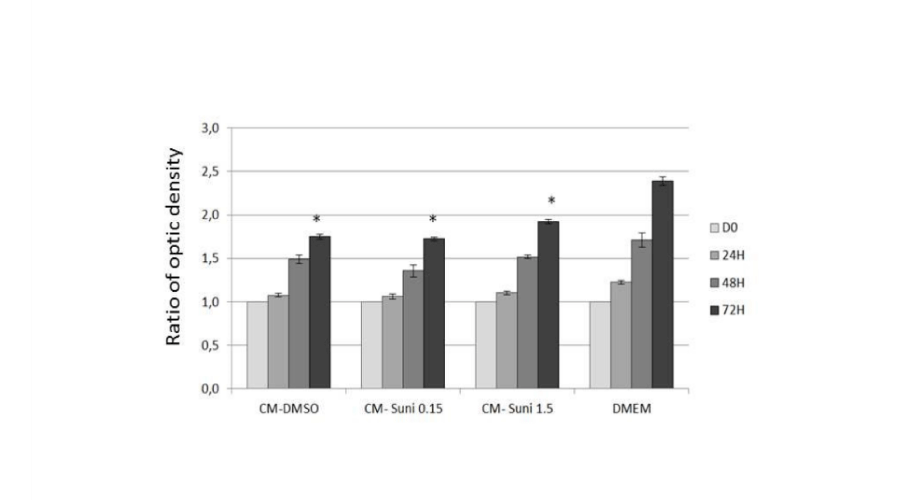
Figure 6:
CM treated-hGVE proliferation by MTT assay. CM corresponds to supernatant of GMVEC culture in EGM2, after treatment by Sunitinib 0.15µM (Suni 0.15) and Sunitinib 1.5µM (Suni 1.5). DMEM is the habitual hGVE culture medium, used as a control. *: p<0.05 compared to DMEM of the same day. Bars and intervals represent the mean ± standard deviation.
Nephrin membrane expression was studied by immunocytochemistry in hGVE cells grown in the presence of CM for 1h, 24h or 48h. After 1h (Figures 7A,C), nephrin extracellular expression (brown staining) was weaker in hGVE cells incubated with CM-Suni (1.5µM) (C) than in cells incubated in CM-DMSO (A). However, after 24h, nephrin expression was stable, in both hGVE cells incubated with CM-DMSO and CM-Suni (1.5µM) (Figures 7B,D). Similar results were obtained by immunofluorescence analysis. Nephrin expression was decreased in hGVE cells incubated with CM-Suni (0.15 and 1.5µM) for 1h (Figures 7F,G) compared with CM-DMSO (Figure 7E). Moreover, in CM-DMSOtreated hGVE cells, nephrin showed predominantly a punctuate perinuclear pattern (arrow) (Figure 7E), whereas CM-Suni treatment induced a redistribution of nephrin expression (F and G). Western blot analysis (Figure 7H) confirmed that nephrin expression was reduced in hGVE cells incubated with CM-Suni in comparison with CM-DMSO or DMSO-treated cells. It also showed that the reduction was proportional to the amount of sunitinib used in GMVEC cells. Moreover, actin distribution also was modified in hGVE cells grown in CM-Suni compared with control cells (CM-DMSO) where actin was organized in filaments along the axis (Figure 8).
-
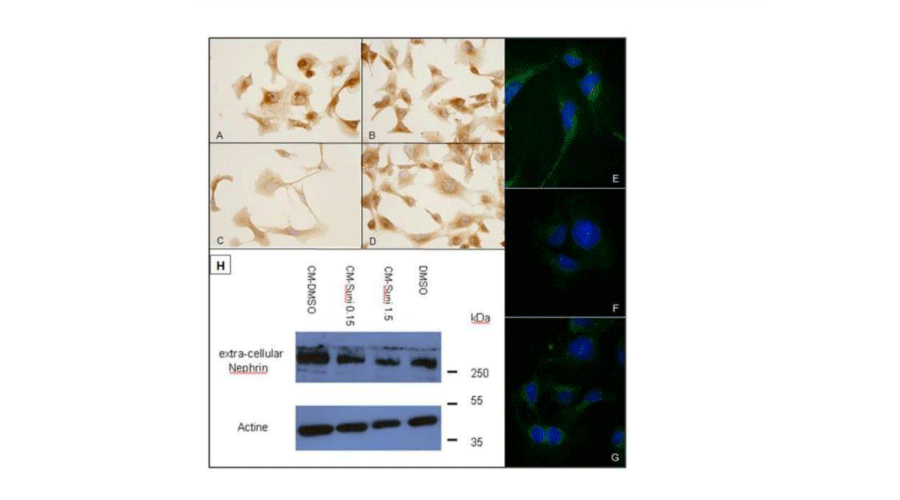
Figure 7:
Nephrin expression by CM-treated hGVE. A to D: extracellular nephrin expression by hGVE treated 1h (A and C) or 24 h (B and D) by CM-DMSO (A and B) or by CM-Sunitinib 1.5µM (C and D), immunocytochemistry. Antinephrin antibody 1/1000. No cell permeabilization. Original magnification x40. E to G: extracellular nephrin expression by hGVE treated 1h by CM-DMSO (E), CMSunitinib 0.15µM (F) or CM-Sunitinib 1.5µM (G) by immunofluorescence. Anti-nephrin antibody 1/1000. Original magnification x40. H: extracellular nephrin expression by hGVE treated 1h by CM-DMSO, CM-Sunitinib 0.15µM, or CM-Sunitinib 1.5µM, by western-blotting. Control DMSO.
-
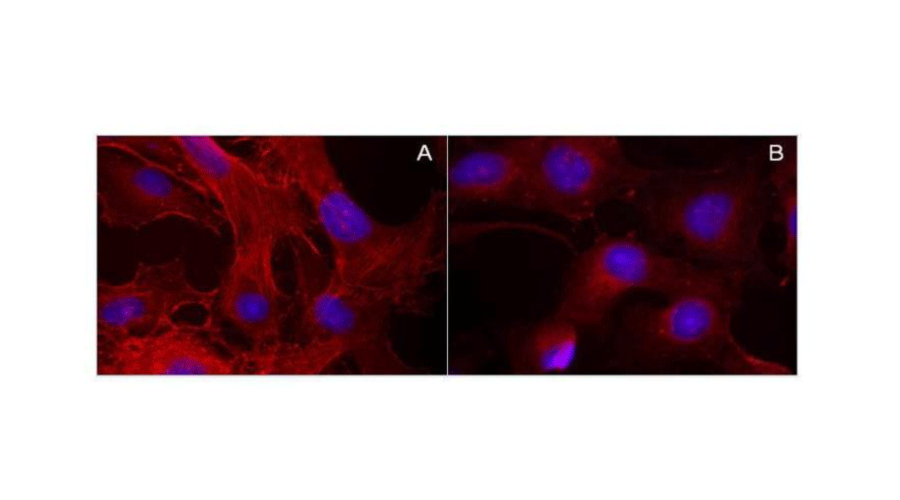
Figure 8:
Actin redistribution in CM-sunitinib-treated hGVE cells. Actin microfilaments stained by phalloidin-rhodamin by immunofluorescence in hGVE treated by CM-DMSO (A) (control) or in hGVE treated by CM-sunitinib 1.5µM (B) during 48h. The incubation with CM did not modify cell viability as detected by tryptan blue dye exclusion. Acquisition time 1000ms (A) and 2000ms (B).
ET-1 role in nephrin expression reduction in CM-treated hGVE cells
As ET-1 was secreted by sunitinib-treated GMVEC cells, we tested whether it was involved in nephrin expression reduction in hGVE cells treated with CM-Suni. To this aim, hGVE cells were pre-incubated with 0.4µM BQ-123 (an ET-RA inhibitor) for 1h before addition of the different CM, as before. Western blotting and immunofluorescence analysis of nephrin membrane expression showed that pre-treatment of hGVE cells with BQ-123 counteracted the effect of CM-Suni on nephrin expression level and cytoplasmic re-distribution (Figure 9; left and right panels, respectively).
-
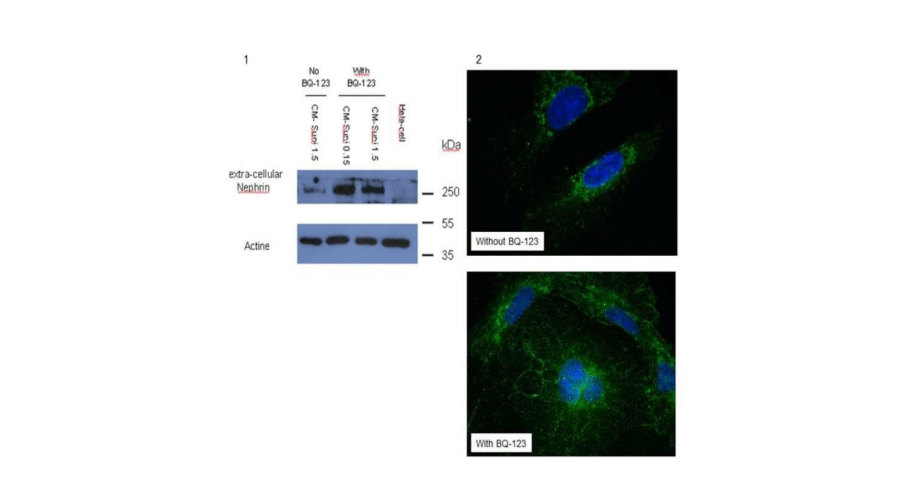
Figure 9:
Pre-treatment of hGVE cells with BQ-123 (endothelin receptor A antagonist) counteracts the effect of CM-Suni on nephrin expression level and cytoplasmic redistribution. By western-blotting (1) and immunofluorescence (2) extracellular nephrin in CM-sunitinib-treated hGVE cells, with or without 1hour pre-treatment by BQ-123 0.4µM
Discussion
Sunitinib is the most used anti-VEGF drug in oncology since 2005. Like with the other therapies targeting the VEGF pathway, its use is associated with glomerular side effects, such as proteinuria and TMA. The molecular mechanisms underlying proteinuria development in patients treated with antiangiogenic therapies have not been much studied. Physiologically, VEGF plays a key role in vascular permeability. In the kidney, podocyte-specific VEGF is essential for the establishment and homeostasis of the glomerular filtration barrier and the fenestrated endothelial capillary system [28] and acts as a paracrine signal via its cellular receptors, including VEGFR-1 (FLT-1), to regulate the slit diaphragm integrity and function [29]. Glomerular permeability requires the proper function of the main slit diaphragm podocyte proteins, particularly nephrin, synaptopodin and podocin. Indeed, mutations in the genes encoding these proteins have been described in patients with proteinuria or nephrotic syndrome [30-32]. In preeclampsia, decreased nephrin expression contributes to damaging the integrity of the glomerular filtration barrier. This could be due to ET-1 action on podocytes, following its release by endothelial glomerular cells [26]. Histologically, TMA lesions and glomerular capillary endotheliosis are observed, with reduced formation of endothelial fenestrae. Similar tissue damage has been recently described in renal biopsies from patients treated with sunitinib. These lesions are associated with decreased expression of synaptopodin, nephrin and podocin in these biopsies and VEGF decrease in all glomeruli [15]. By analogy with preeclampsia, it has been hypothesized that nephrin expression could be modulated by endothelin following sunitinib-mediated promotion of its secretion by endothelial cells.
To our knowledge, this is the first study that evaluated in vitro sunitinib effects on cells of the glomerular filtration barrier. We used hGVE cells that are derived from podocytes and GMVEC. First, we analyzed cell proliferation/viability to assess sunitinib cytotoxicity and establish the sunitinib doses to be used for the subsequent experiments. Cytotoxicity was important at high sunitinib doses, particularly after four days of treatment (the only experiment carried out over four days). Thus, when used at high supra-therapeutic doses, sunitinib is cytotoxic for both epithelial and endothelial glomerular cells. In the clinical practice, the renal side effects of anti-angiogenic drugs are not immediate, but appear during the patient follow-up and seem to be cumulative and dose-dependent. Sometimes, lower dose treatment allows continuing the treatment with sunitinib by decreasing proteinuria or reducing hypertension [33]. It is thus possible that more effects would have been observed with longer incubation times.
We then show that sunitinib has a direct effect on GMVEC cells. Conversely, in hGVE cells its effects are mainly indirect (but for the effect on cell viability/proliferation) through endothelial cells. In support of endothelin role, this anti-VEGF treatment stimulated ET-1 production by GMVEC cells. Moreover, sunitinib led to VE-cadherin disorganization at the cell membrane. We confirmed that sunitinib does not have any direct effect on nephrin expression or on the ET-1 system in hGVE cells. Conversely, when hGVE cells were cultured in the presence of CM from sunitinib-treated GMVEC cells, nephrin expression was reduced. As several mediators have been reported to affect nephrin expression/localization by activation of the cell cytoskeleton and by cleavage of the extracellular domain of nephrin [34], we also investigated actin organization in hGVE cells incubated with CM and found that actin distribution was affected only in cells grown in CM-Suni. We can hypothesize that activation of the cell cytoskeleton modifies nephrin surface expression because total nephrin expression was not altered. Moreover, our findings highlight the role of ET-RA in nephrin decrease and cytoskeleton activation because pre-incubation with an antagonist of this receptor blocked the effects of CM-Suni. The therapeutic potential of endothelin antagonists has already been studied in some renal diseases, such as glomerulosclerosis or diabetic nephropathy [35], and our results suggests that they could be useful also for the renal side effects of antiangiogenic targeted therapies.
Conclusion
In vitro sunitinib shows dose-dependent toxicity in GMVEC cells (a human glomerular endothelial cell model) and in hGVE cells (a human podocyte model). At high doses, it inhibits cell proliferation and reduces cell viability. Sunitinib does not directly perturb slit diaphragm protein expression in hGVE cells. Conversely, in GMVEC cells, it stimulates ET-1 production and secretion and leads to VE-cadherin disorganization. Sunitinib effects on slit diaphragm proteins seem to be indirect through the action of GMVEC-released ET-1 on ET-RA in hGVE cells. The blockage of sunitinib-induced modifications by endothelin-receptor inhibitors is a very important result for future clinical practice. Indeed, endothelia inhibitors are available and could represent a therapeutic option for the renal side effects of anti-angiogenic drugs in patients with cancer.
-
-
- Albiges L, Salem M, Rini B, Escudier B (2011) Vascular endothelial growth factor-targeted therapies in advanced renal cell carcinoma. Hematol Oncol Clin North Am 25: 813–833.
- Fan F, Schimming A, Jaeger D, Podar K (2012) Targeting the tumor microenvironment: focus on angiogenesis. J Oncol 2012: 281261.
- Escudier B, Eisen T, Stadler WM, Szczylik C, Oudard S, et al. (2007) Sorafenib in advanced clear-cell renal-cell carcinoma. N Engl J Med 356: 125–134.
- Motzer RJ, Hutson TE, Tomczak P, Michaelson MD, Bukowski RM, et al. (2007) Sunitinib versus interferon alfa in metastatic renal-cell carcinoma. N Engl J Med 356: 115-124.
- Motzer RJ, Hutson TE, Tomczak P, Michaelson MD, Bukowski RM, et al. (2009) Overall survival and updated results for sunitinib compared with interferon alfa in patients with metastatic renal cell carcinoma. J Clin Oncol 27: 3584–3590.
- Patard J-J, Pignot G, Escudier B, Eisen T, Bex A, et al. (2011) ICUD-EAU International Consultation on Kidney Cancer 2010: treatment of metastatic disease. Eur Urol 60: 684–690.
- Izzedine H, Massard C, Spano JP, Goldwasser F, Khayat D, et al. (2010) VEGF signalling inhibition-induced proteinuria: Mechanisms, significance and management. Eur J Cancer 46: 439–448.
- Winn SK, Ellis S, Savage P, Sampson S, Marsh JE (2009) Biopsy-proven acute interstitial nephritis associated with the tyrosine kinase inhibitor sunitinib: a class effect? Nephrol Dial Transplant 24: 673–675.
- Costero O, Picazo ML, Zamora P, Romero S, Martinez-Ara J, et al. (2010) Inhibition of tyrosine kinases by sunitinib associated with focal segmental glomerulosclerosis lesion in addition to thrombotic microangiopathy. Nephrol Dial Transplant 25: 1001–1003.
- Thariat J, Janus N, Barrière J, Launay-Vacher V (2012) [Renal tolerance of targeted therapies]. Bull Cancer 99: 317–322.
- Bollée G, Patey N, Cazajous G, Robert C, Goujon J-M, et al. (2009) Thrombotic microangiopathy secondary to VEGF pathway inhibition by sunitinib. Nephrol Dial Transplant 24: 682–685.
- Eremina V, Jefferson JA, Kowalewska J, Hochster H, Haas M, et al. (2008) VEGF inhibition and renal thrombotic microangiopathy. N Engl J Med 358: 1129–1136.
- Frangié C, Lefaucheur C, Medioni J, Jacquot C, Hill GS, et al. (2007) Renal thrombotic microangiopathy caused by anti-VEGF-antibody treatment for metastatic renal-cell carcinoma. The Lancet Oncology 8: 177–178.
- Sugimoto H, Hamano Y, Charytan D, Cosgrove D, Kieran M, et al. (2003) Neutralization of circulating vascular endothelial growth factor (VEGF) by anti-VEGF antibodies and soluble VEGF receptor 1 (sFlt-1) induces proteinuria. J Biol Chem 278: 12605–12608.
- Vigneau C, Lorcy N, Dolley-Hitze T, Jouan F, Arlot-Bonnemains Y, et al. (2014) All antivascular endothelial growth factor drugs can induce “pre-eclampsia-like syndrome”: a RARe study. Nephrol Dial Transplant 29: 325–332.
- Henao DE, Saleem MA, Cadavid AP (2010) Glomerular disturbances in preeclampsia: disruption between glomerular endothelium and podocyte symbiosis. Hypertens Pregnancy 29: 10–20.
- Vuorela P, Helske S, Hornig C, Alitalo K, Weich H, et al. (2000) Amniotic fluid--soluble vascular endothelial growth factor receptor-1 in preeclampsia. Obstet Gynecol 95: 353–357.
- Maynard SE, Min J-Y, Merchan J, Lim K-H, Li J, et al. (2003) Excess placental soluble fmslike tyrosine kinase 1 (sFlt1) may contribute to endothelial dysfunction, hypertension, and proteinuria in preeclampsia. J Clin Invest 111: 649–658.
- Zhao J, Gu Y, Fan R, Groome LJ, Wang Y (2011) Factors derived from preeclamptic placentas perturb polarity protein PARD-3 expression and distribution in endothelial cells. Reprod Sci 18: 164–171.
- Esser S, Lampugnani MG, Corada M, Dejana E, Risau W (1998) Vascular endothelial growth factor induces VE-cadherin tyrosine phosphorylation in endothelial cells. J Cell Sci 111: 1853–1865.
- Müller-Deile J, Schiffer M (2011) Renal involvement in preeclampsia: similarities to VEGF ablation therapy. J Pregnancy 2011: 176973.
- Cazaubon S, Deshayes F, Couraud P-O, Nahmias C (2006) [Endothelin-1, angiotensin II and cancer]. Med Sci (Paris) 22: 416–422.
- Kappers MHW, van Esch JHM, Sluiter W, Sleijfer S, Danser AHJ, et al. (2010) Hypertension induced by the tyrosine kinase inhibitor sunitinib is associated with increased circulating endothelin-1 levels. Hypertension 56: 675–681.
- Kappers MHW, Smedts FMM, Horn T, van Esch JHM, et al. (2011) The vascular endothelial growth factor receptor inhibitor sunitinib causes a preeclampsia-like syndrome with activation of the endothelin system. Hypertension 58: 295–302.
- Roselli S, Gribouval O, Boute N, Sich M, Benessy F, et al. (2002) Podocin localizes in the kidney to the slit diaphragm area. Am J Pathol 160: 131–139.
- Collino F, Bussolati B, Gerbaudo E, Marozio L, Pelissetto S, et al. (2008) Preeclamptic sera induce nephrin shedding from podocytes through endothelin-1 release by endothelial glomerular cells. Am J Physiol Renal Physiol 294: F1185–1194.
- Delarue F, Virone A, Hagege J, Lacave R, Peraldi MN, et al. (1991) Stable cell line of T-SV40 immortalized human glomerular visceral epithelial cells. Kidney Int 40: 906–912.
- Eremina V, Baelde HJ, Quaggin SE (2007) Role of the VEGF--a signaling pathway in the glomerulus: evidence for crosstalk between components of the glomerular filtration barrier. Nephron Physiol 106: 32–37.
- Ferrara N, Gerber H-P, LeCouter J (2003) The biology of VEGF and its receptors. Nat Med 9: 669–676.
- Kestilä M, Lenkkeri U, Männikkö M, Lamerdin J, McCready P, et al. (1998) Positionally cloned gene for a novel glomerular protein--nephrin--is mutated in congenital nephrotic syndrome. Mol Cell 1: 575–582.
- Boute N, Gribouval O, Roselli S, Benessy F, Lee H, et al. (2000) NPHS2, encoding the glomerular protein podocin, is mutated in autosomal recessive steroid-resistant nephrotic syndrome. Nat Genet 24: 349–354.
- Dai S, Wang Z, Pan X, Wang W, Chen X, et al. (2010)Functional analysis of promoter mutations in the ACTN4 and SYNPO genes in focal segmental glomerulosclerosis. Nephrol Dial Transplant 25: 824–835.
- Takahashi D, Nagahama K, Tsuura Y, Tanaka H, Tamura T (2012) Sunitinib-induced nephrotic syndrome and irreversible renal dysfunction. Clin Exp Nephrol 16: 310–315.
- Doublier S, Salvidio G, Lupia E, Ruotsalainen V, Verzola D, et al. (2003) Nephrin expression is reduced in human diabetic nephropathy: evidence for a distinct role for glycated albumin and angiotensin II. Diabetes 52: 1023–1030.
- Rafnsson A, Böhm F, Settergren M, Gonon A, Brismar K, et al. (2012) The endothelin receptor antagonist bosentan improves peripheral endothelial function in patients with type 2 diabetes mellitus and microalbuminuria: a randomised trial. Diabetologia 55: 600–607.
-
-
-
-
-
-









Table 1:
Primary antibodies used in Western-blot, immunofluorescence or immunocytochemistry.