Authors:
Benjamin Chitambira1* and David Smithard2
1Richard Stevens Stroke Unit, Physiotherapy Department, East Kent Hospitals University NHS Foundation Trust, UK
2Princess Royal University Hospital, King’s College Hospital NHS Foundation Trust, UK
Received: 02 September, 2015;Accepted: 03 October, 2015; Published: 05 October, 2015
Benjamin Chitambira, Richard Stevens Stroke Unit, Physiotherapy Department, East Kent Hospitals University NHS Foundation Trust, William Harvey Hospital, Kennington Road, Ashford, Kent, UK, TN24 0LZ, Tel: 00441233616242; E-mail:
Chitambira B, Smithard D (2015) Exploring the Extent of Restoration of Voluntary Movements, Function, Quality of Life and Cost of Formal Care in Dense Strokes Treated by the Optokinetic Chart Stimulation Based OKCSIB Protocol: A Prospective Pilot Randomised Case Controlled Study. J Nov Physiother Phys Rehabil 2(2): 051-057. DOI: 10.17352/2455-5487.000025
© 2015 Chitambira B, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Optokinetic chart stimulation; Neuro physiotherapy; Neuro rehabilitation; Dense acute stroke; Limb recovery
Background: Stroke remains one of the largest causes of impairment and disability globally. Stroke involves high costs to the health economy.
Objective: To explore the extent of recovery of voluntary movements and function in dense acute strokes treated with the optokinetic chart stimulation based OKCSIB protocol.
Methods: The experimental patient was treated with the OKCSIB protocol. An optokinetic chart was moved in front of the patient for 3 minutes each of lateral, vertical and forwards, twice daily for 5 days a week. The control patient underwent conventional therapy which involved practicing functional task with facilitation of normal movements as per Bobath approach. The main outcome measure was the STREAM upper and lower limb score after 14 weeks.
Results: The experimental patient’s upper limb STREAM scores improved from 0/20 pre-treatment to 18/20 after 14 weeks and 20/20 after 3 months follow up. The control patient’s upper limb STREAM score remained 0/20 pre-treatment, 0/20 after 14 weeks and 0/20 after 3 months follow up. The experimental patient’s lower limb STREAM scores improved from 0/20 pre-treatment to 20/20 after 14 weeks and 20/20 after 3 months follow up. The control patient’s lower limb STREAM score remained 0/20 pre-treatment, 0/20 after 14 weeks and 0/20 after 3 months follow up. The experimental patient’ s function improved from Barthel Index score of 0/20 pre-treatment to 17/20 after 14 weeks and 18/20 after 3 months follow up. The control patient scored 0/20 pre-treatment, 1/20 after 14 weeks and 0/20 after 3 months follow up.
Conclusions: The OKCSIB protocol restored voluntary movements and function when compared to conventional therapy. Fully powered studies are recommended to test the efficacy of the OKCSIB protocol against conventional neuro physiotherapy.
Introduction
Stroke remains as one of the most devastating of all neurological diseases [1]. It often leads to physical impairment, disability and death [1]. Stroke exerts a huge strain on the health economy when its treatment, rehabilitation, social care and loss of productivity are considered. It costs 8.9 billion pounds in the UK [2] and 34.3 billion dollars in the US [3]. In stroke patients, functional independence and daily life autonomy are correlated to trunk function, upper limb impairment [4], arm recovery [5] and extensor strength in the affected upper limb [6]. A third of stroke patients develop spasticity of the affected upper limb [7]. In sub-acute stroke patients, walking speed is decreased by weakness of the affected lower limb’s anti-gravity extensor muscles such as hip abductors, hip extensors and knee extensors [8].
A systematic review has shown that the widely used Bobath approach has no evidence for recovery of movements and function in strokes [9]. A recent review has shown that of all conventional neurophysiotherapy approaches, no single conventional neurophysiotherapy approach is superior to any of the other conventional neurophysiotherapy approaches for recovery of function and mobility after stroke [10]. Most conventional neurorehabilitation aims for compensatory function with little time given for upper limb recovery [11]. Even with the move towards repetitive task specific training, it has been shown that people with dense strokes cannot tolerate the high intensities required [12]. This usually involves repeatedly practicing the same functional task for 2 to 4 hours daily at least 5 days a week. Still, upper limbs do not benefit enough to recover movements from upper limb training [13]. Thus it is important to find efficient rehabilitation interventions that improve upper limb and lower limb recovery as well as reduce spasticity in dense acute strokes.
Optokinetic chart stimulation (OKCS) is a novel intervention for neurorehabilitation of completely hemiplegic acute strokes [14-16]. The optokinetic chart is designed on A4 paper and consists of repeated groups of lines with the colours red, orange, yellow, green, blue, indigo and violet. The chart is kept at a distance of 15 to 20 centimeters from the patient’s face and then moved from side to side at approximately one cycle per second for 3 minutes. This is followed by moving the chart up and down for 3 minutes and then forwards and backwards for another 3 minutes. All the patient does is look at the centre of the chart. OKCS is carried out on its own until a patient can stand in parallel bars with the assistance of 2 therapists. At this point sensory interaction for balance (SIB) by standing on balance pads for 3 minutes, is added. This is how the intervention protocol derived the acronym, OKCSIB. It was designed as a further development to the evidence from small trials which showed that optokinetic stimulation had benefits in the treatment of neglect in stroke patients [17]. A novel OKCSIB protocol [15,16], based on OKCS, had its efficacy incrementally assessed through a case series [15] and then a case control series [16]. The preliminary evidence from these studies warranted further assessment of the benefits of the OKCSIB protocol under randomized controlled trial conditions. The objective of the study is to explore the difference in the extent of restoration of voluntary movements, function, quality of life and weekly cost of formal care between dense acute strokes treated by the OKCSIB protocol and those treated by conventional neurophysiotherapy which involved practicing functional tasks with facilitation of normal movements as per Bobath approach.
Methods
Design, setting and ethics
The design was a single blind pilot randomized controlled trial in a combined hyper-acute and rehabilitation stroke unit setting. Ethical approval was given by the London-Surrey Borders Research Ethics Committee. Written informed consent was obtained from each participant. The study’s international trials registry number is ISRCTN35657537.
Methodology
Potential participants, aged between 75 years and 85 years, and had dense strokes that completely paralysed the affected upper and lower limbs, were recruited into the study. They were recruited if they were able to provide consent. Participants were assigned to either the OKCSIB group or the conventional neurophysiotherapy group by blind remote block randomisation. Table 1 shows the selection criteria for the study.
The experimental intervention was the OKCSIB protocol [15]. The optokinetic chart is designed on A4 paper and consists of repeated groups of lines with the colours red, orange, yellow, green, blue, indigo and violet. The chart was kept at a distance of 15 to 20 centimetres from the patient’s face and then moved from side to side at approximately one cycle per second for 3 minutes. This was followed by moving the chart up and down for 3 minutes and then forwards and backwards for another 3 minutes. All the participant did was look at the centre of the chart. This is done twice daily for 5 days per week. Once a patient could stand with assistance of 2 therapists in parallel bars, sensory interaction for balance (SIB) was added with the participant standing on a balance pad for 3 minutes [14-16]. For the affected upper limb active-assisted anti-gravity extensor exercises were carried out as follows: 5 repetitions for each of shoulder external rotation, shoulder abduction, shoulder flexion and then of a combination of these movements in the proprioceptive neuromuscular facilitation (PNF) pattern of D2F, elbow extension, wrist supination, wrist extension and fingers extension [14,15].
The OKCSIB protocol is progressed by adding backwards and sideways stepping when participants have improved to mobilising in parallel bars with assistance of two therapists [15]. This is to challenge cortico-midbrain locomotors area- lateral vestibulospinal descending motor network [22] for proximal anti-gravity extensor control. On most days the OKCSIB protocol was carried out by the first author. Conventional activities of daily living that the participant could do as they progressed were added to the OKCSIB protocol. The OKCSIB protocol was carried out daily for 5 days per week for 14 weeks.
The control intervention was carried out and supervised by a conventional physiotherapist trained in the Bobath based normal movement approach. This consisted of facilitation of normal movement patterns and conventional activities of daily living. Both the experimental and control participants received the same occupational therapy concurrently as deemed suitable by their occupational therapists.
Outcome measurement
The outcome measures were scored by a blinded neurophysiotherapist who carried out the measurements at the participant’s places of residence at the time of measurement. Validated questionnaires were used to measure the outcomes after 14 weeks. The intervention period was 14 weeks. Participants were then followed up to reassess outcomes after 3 months from the 14 weeks. It took 2 hours to complete the questionnaires per each testing session. The primary outcome measure is the Stroke Rehabilitation Assessment of Movement (STREAM) upper and lower limb scores at 14 weeks. STREAM scores after 8 weeks and after 3 months follow up were also used as secondary outcome measures. STREAM is a validated impairment measure [18] with a maximum score of 20 for each of the affected limbs and a maximum total score of 70 when the mobility subsection is included. Other secondary outcome measures included the Barthel Index [19] after 8 weeks, 14 weeks and 3 months follow up; the modified Ashworth Scale (MAS) [20] and the Stroke Specific Quality of Life (SSQOL) [21] after 14 weeks and 3 months follow up. The Barthel Index is a validated measure of activities of daily living with a maximum score of 20. The MAS and SSQOL are valid measures of spasticity and quality of life respectively with respective maximum scores of 5 and 245. The weekly cost of formal care (WCFC) was also used as a secondary outcome measure after the 3 months follow up. The outcome measurements were carried out by a blinded physiotherapist who did not work in the researcher’s organization.
Results
A total of 216 potential participants were screened for eligibility over a period of 13 months. Figure 1 shows the CONSORT diagram for the study. Only 4 participants were eligible and these were recruited into the study. Out of the 4, one was withdrawn after she was repatriated out of the catchment area and one died from a medical complication unrelated to the study. Two participants completed the study. The experimental participant was a female aged 77 whilst the control participant was a female aged 78. In terms of CT scan reports, the experimental participant had an extensive right fronto-parieto-occipital infarct and the control participant had a left basal ganglia infarct. The experimental participant had unilateral spatial neglect whilst the control participant did not. From those potential participants that had dense weakness, recruitment was limited by the inability to consent and the tightly controlled age range. Figure 1 shows the CONSORT flow chart for the study.
-
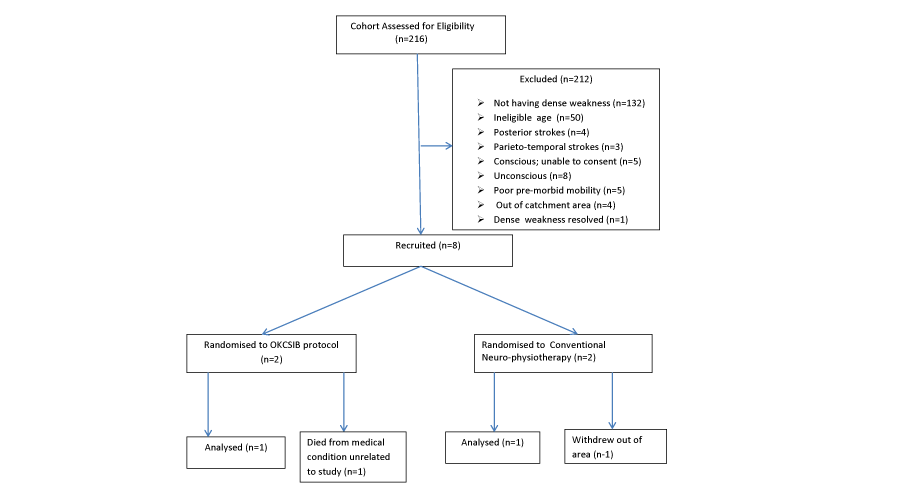
Figure 1:
Consort flow diagram for the pilot study.
The experimental participant had fully recovered affected upper and lower limb movements by the 3 months follow up. The 3 months follow up was carried out after 6 months from date of randomization. On the other hand, the control participant did not recover voluntary movements of the affected upper and lower limbs at all. Instead, by the 3 months follow up, the control participant had developed spasticity of the affected hand and affected lower limb. The control participant’s affected lower limb was already in a flexor pattern of hip abduction, flexion and external rotation with knee flexion.
The control participant was discharged to a nursing home with use of hoists for transfers. The experimental participant returned home and was independently mobile outdoors and only privately paid a carer to help with cleaning her bungalow.
Table 2 shows the detailed results for all outcome measures. The bar charts comparing experimental versus control STREAM scores are shown in Figure 2. Figure 3 shows the comparisons of the experimental and control Barthel Index and MAS scores. The SSQOL and WCFC scores are shown in Figure 4. Figure 5 shows the trajectory of recovery of voluntary movements throughout the measurement timelines.
-

Table 2:
Outcomes after 8 weeks, 14 weeks and 3 month follow up.
-
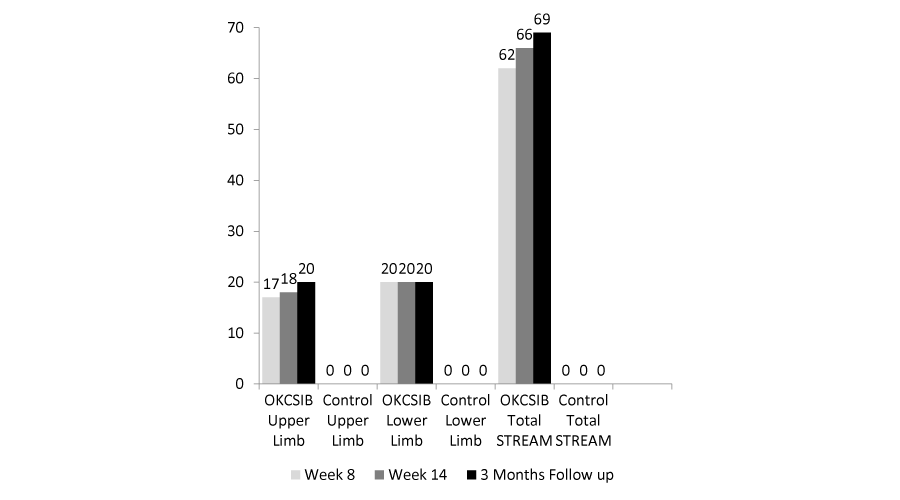
Figure 2:
Upper and lower limb STREAM scores and total STREAM scores for the experimental OKCSIB protocol participant and the conventional neurophysiotherapy control participant respectively.
-

Figure 3:
Barthel Index and modified Ashworth Scale scores for the OKCSIB protocol participant and conventional neurophysiotherapy participant respectively.
-
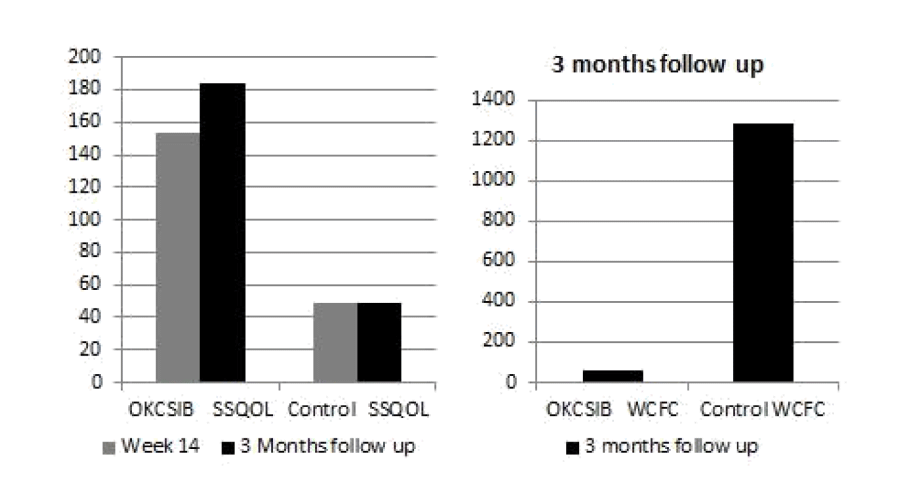
Figure 4:
Stroke Specific Quality of Life (SQOL) and weekly cost of formal care (WCFC)scores for the OKCSIB protocol and control conventional neurophysio therapy participants respectively.
-
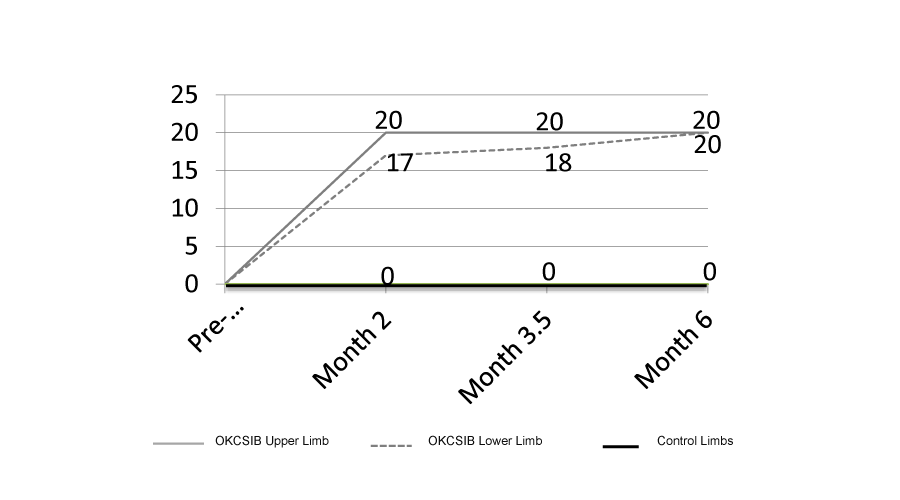
Figure 5:
Recovery trajectories for the OKCSIB and control participants respectively.
Discussion
The OKCSIB protocol participant had full recovery of the affected upper and lower limbs by the 3 months follow up. On the other hand the control conventional neurophysiotherapy participant did not recover any voluntary movements. The OKCSIB protocol participant also recovered function whereas the conventional neurophysiotherapy control participant had lost all function by the 3 months follow up. In terms of spasticity, only the control participant developed spasticity of the affected hand. The OKCSIB protocol participant had better quality of life. The control participant cost more than a thousand pounds per week for formal care when compared to the OKCSIB protocol participant. These incremental results add on to the evidence from the case control series that found the OKCSIB protocol to lead to better recovery of affected upper limbs and prevention of hand spasticity [16].
This study is the first preliminary randomized case controlled prospective study of the extent of recovery of voluntary movements and function between the OKCSIB protocol and conventional neurophysiotherapy. The full recovery of the affected upper limb for the OKCSIB participant is significant as even with the currently best evidence based repetitive task specific training approach, there remains little evidence for upper limb recovery [23]. This is important as functional autonomy is known to be correlated with upper limb recovery [4-6]. Out of the two participants only the OKCSIB protocol participant had visuospatial neglect pre-treatment. From evidence on the impact of neglect in dense strokes [24], the OKCSIB protocol participant would have been the one expected to be severely disabled, with little prospect for recovering the affected upper limb. On the contrary, it is the control participant who had no neglect who failed to recover the affected upper and lower limb as well as function.
With the OKCSIB protocol, focal basal ganglia infarcts recover full use of their affected limbs [15]. Thus the control participant would have been expected to recover use of the affected limbs if treated by optokinetic chart stimulation. Instead the control participant has spastic affected upper and lower limbs and is fully dependent on sling hoists and carers for all functions.
Most stroke research studies have concentrated on patients with residual minimal movements and have no evidence for recovery of completely paralysed dense strokes [24]. On the other hand the OKCSIB protocol’s evidence is based on dense completely paralysed strokes with no residual movements. This is especially important given the fact that functional independence depends on recovery of the upper limb [25]. The recovery of lower limbs is also significant as it enables regaining of independent mobility with a normal gait and walking speed [8]. The fact that the recovery of voluntary movements starts to plateau after 8 weeks of the OKCSIB protocol intervention reinforces the findings of the OKCSIB protocol case series [15]. Recovery peaked at 3 months for the OKCSIB protocol intervention and this confirms similar findings by studies which show that the best window for recovery after stroke is within the first 3 months [26,27]. This pilot study plays an important role in sign posting future studies into recovery of impairments so as to delineate intervention effects from spontaneous recovery [24]. It is a preliminary step towards finding efficient recovery interventions for the acute to sub-acute phases of stroke. This is important because overall functional compensatory rehabilitation may lead to poor recovery due to aberrant plasticity of the affected side [28]. In the chronic stages of stroke there is more of compensation occurring rather than recovery [29].
Networks responsible for voluntary movements include primary motor cortex, lateral premotor cortex and supplementary motor area, as well as in subcortical areas such as basal ganglia, thalamus, cerebellum, brainstem nuclei [30], and fronto-parietal areas [31,32]. Optokinetic stimulation is known to stimulate cerebral cortical areas in the temporo-parietal regions, thalamus, basal ganglia [33], brain stem and cerebellum [34]. These areas of the brain are important for voluntary movements, balance and co-ordination. Without recovery of these networks, functional gains would be mostly compensatory. However compensation is very difficult to achieve for dense strokes with complete hemiplegia. These strokes have cortico-midbrain locomotor area-vestibulospinal networks [22] which maintain anti-gravity extensor control that are severely disrupted and they end up with loss of reciprocal inhibition of flexors. This then leads to flexors tightening, with contractures developing as spasticity sets in.
The OKCSIB protocol is a balance and co-ordination system recovery focused intervention [15,16] which addresses the finding that the key feature of stroke that determines severity of disability is balance [35] or postural control [36]. Abnormal multisensory integration is a known problem in stroke patients [37]. The authors propose that the main mechanism of OKCS is the visuospatial disorientation which enhances recovery of networks that are important for multisensory integration, balance and spatial orientation. This results in recovery to improve the multimodal vestibular system [38] which in turn improves proximal anti-gravity extensor control in the upper limbs and lower limbs [22].
Other approaches have high intensities and go on for long into the chronic phases when compared to the OKCSIB protocol which only takes 25 minutes daily for 5 days per week [14,15]. This is important as most acute stroke unit patients tend to have severe disability and are less likely to participate in intense neurophysiotherapy and thus fall short of the guideline intensity [39] of a minimum of 45 minutes daily [40].
The study has been limited by the small number of participants as potential participants who were unable to consent were excluded. Most dense strokes tend to have cognitive and or communication difficulties. It is proposed that future trials include participants who may be unable to consent but are able to express an interest in the study as long as they have a legal advocate to assent for their informed consent. The effect size of the OKCSIB protocol is very clinically significant and has complete versus no recovery. This is in keeping with anecdotal clinical observations. Such a major difference in effect size if reproduced in a full trial would fulfil the all and none principle of an ideal scientific experiment.
It is recommended that full randomized controlled trials be carried out in completely paralyzed acute strokes, as the damage to networks is enough to minimize effects of natural spontaneous recovery. Full trials are also recommended to compare the extent and speed of recovery in acute stroke patients with hemiparesis. The authors also propose that future research with optokinetic chart stimulation and other forms of optokinetic stimulation should investigate neuro-radiological and biochemical correlates of the observed recovery of impairments.
Conclusion
Optokinetic chart stimulation has the potential to lead to remarkable recovery of voluntary movements and function in dense parietal centred acute strokes when compared to conventional neurophysiotherapy. More research is needed to confirm the potential benefits of the intervention.
Acknowledgements
Acknowledgements go to the patients who consented to take part in the study. The authors acknowledge the invaluable role played by Mr Tony Pellicci and Mrs Marilyn Pellicci as lay members of the steering committee. Linda Cowie and Barbara Ransom are acknowledged for the remote block randomisation. Acknowledgement is also given to Charlotte Jeffery, the therapy support worker who assisted with carrying out optokinetic chart stimulation. Mary Mukutuma is also acknowledged for carrying out the blinded outcome assessments.
-
-
- Mukherjee D, Patil CG (2011) Epidemiology and the global burden of stroke. World Neurosurg 76: S85-S90.
- Saka O, McGuire A, Wolfe C (2009) Cost of stroke in the United Kingdom. Age and Aging 38: 27-32.
- Centers for Disease Control and Prevention (CDC) (2012) Prevalence of Stroke – United States, 2006-2010. MMWR 61: 379-382.
- Likhi M, Jidesh VV, Kanagaraj R, George JK (2013) Does trunk, arm, or leg control correlate best with overall function in stroke subjects? Topics in Stroke Rehabilitation 20: 62-67 .
- Smania N, Gambarin M, Tinazz IM, Picelli A, Fiaschi A, et al. (2009) Are indexes of arm recovery related to daily life autonomy in patients with Eur J Phys Rehabil Med 45: 349-354.
- Turk R, Burridge JH, Simpson DM (2012) Motor impairments associated with loss of upper limb functional activity early and late post-stroke. Neurorehabil and Neural Repair 26: S751.
- Rosales RL, Kanovsky P, Fernandez HH (2011) What’s the “catch” in upper-limb post-stroke spasticity: Expanding the role of botulinum toxin applications. Parkinsonism Relat Disord17: S3-S10.
- BrincksJ, Nielsen JF (2012) Increased power generation in impaired lower extremities correlated with changes in walking speeds in sub-acute stroke patients. Clin Biomech 27: 138-144 .
- Kollen BJ, Lennon S, Lyons B, Wheatley-Smith L, Scheper M, et al. (2009) The effectiveness of the Bobath concept in stroke rehabilitation: What is the evidence. Stroke 40: e89-97.
- Pollock A, Baer G, Pomeroy VM, Langhorne P (2014) Physical rehabilitation approaches for the recovery of function and mobility following stroke. Cochrane Database of Syst Rev 4: 1469493X.
- Hayward KS, Brauer SG (2014) Stroke survivors are engaged in limited upper limb training: A systematic review. Stroke 45: e290.
- Aldred J (2014) Does intensity of physiotherapy in the acute stroke unit depend on stroke severity? International Journal of Stroke 9: 1747-4930.
- Byoung-Jin J, Won-Ho K, Eun-Young P (2014) Effect of task-oriented training for people with stroke: A meta-analysis focused on repetitive or circuit training. Top Stroke Rehabil 22: 34-43.
- Chitambira B (2009) A case report on the use of a novel optokinetic chart stimulation intervention for the restoration of voluntary movement and mobility in a patient with an acute hemorrhagic stroke. NeuroRehabilitation 25: 251-254 .
- Chitambira B (2011) Use of an optokinetic chart stimulation intervention for restoration of voluntary movement, postural control and mobility in acute stroke patients and one post intensive care polyneuropathy patient: A case series. NeuroRehabilitation 28: 99-104 .
- Chitambira B (2014) Does use of the optokinetic chart stimulation based OKCSIB protocol improve recovery of upper and lower limb movements, function and quality of life at 3 year follow up in dense strokes? A retrospective case control series. NeuroRehabilitation 35: 451–458.
- Kerkhoff G, Keller I, Artinger F, Hildebrandt H, Marquardt C, et al. (2012) Recovery from auditory and visual neglect after optokinetic stimulation with pursuit eye movements–transient modulation and enduring treatment effects. Neuro psychologia 50: 1164-1177 .
- Hsieh Y-W, Wang C-H, Sheu C-F, Hsueh I-P, Hsieh CL (2008) Estimating the minimal clinically important difference of the stroke rehabilitation assessment of movement measure. Neurorehabil Neural Repair 22: 723-727.
- Duffy L, Gajree S, Langhorne P, Stott DJ, Quinn TJ (2013) Reliability [inter-rater agreement] of the Barthel Index for assessment of stroke survivors: Systematic review and meta-analysis. Stroke 44: 462-468.
- Kaya T, Karatepe AG, Gunaydin R, Koc A, Altundal Ercan U (2011) Inter-rater reliability of the Modified Ashworth Scale and modified Modified Ashworth Scale in assessing post stroke elbow flexor spasticity. Int J Rehabil Res 34: 59-64.
- Lin KC, Fu T, Wu CY, Hsieh CJ (2011) Assessing the Stroke-Specific Quality of Life for outcome measurement in stroke rehabilitation: Minimal detectable change and clinically important difference. Health and Quality of Life Outcomes 9: 5.
- Elbe RJ, Kattah JC (2012) Approach to the patient with gait disturbances and recurrent falls. In J. Biller [Ed.], Practical Neurology. Philadelphia, USA: Lippincott Williams & Wilkins
- Schaefer SY, Chavelle BP, Lang CE (2013) Transfer of training between distinct motor tasks after stroke: Implications for task-specific approaches to upper-extremity neurorehabilitation. Neurorehabil Neural Repair 27: 602-612.
- Nijboer TCW, Kollen BJ, Kwakkel G (2014) The Impact of Recovery of Visuo-Spatial Neglect on Motor Recovery of the Upper Paretic Limb after Stroke. PLoS ONE 9: e100584 .
- Stinear CM, Petoe MA, Anwar S, Barber PA, Byblow WD (2014) Bilateral priming accelerates recovery of upper limb function after stroke: a randomized controlled trial. Stroke 45: 205-210.
- Wade DT, Wood VA, Hewer RL (1985) Recovery after stroke—the first 3 months. J Neurol Neurosurg Psychiatry 48: 7-13 .
- Krakauer JW, Carmichael ST, Corbett D, Wittenberg GF (2012) Getting Neurorehabilitation Right: What Can Be Learned From Animal Models? Neurorehabilitation and Neural Repair 26: 923 –931 .
- Kim SY, Allred RP, Adkins DL, Tennant KA, Donlan NA, et al. (2015) Experience with the “Good” Limb Induces Aberrant Synaptic Plasticity in the Peri-lesion Cortex after Stroke. J Neurosci 35: 8604-8610.
- Kitago T, Liang J, Huang VS, Hayes S, Simon P, et al. (2013) Improvement after constraint-induced movement therapy: recovery of normal motor control or task-specific compensation? Neurorehabil Neural Repair 27: 99-109 .
- Middleton FA, Strick PL (2000) Basal ganglia and cerebellar loops: motor and cognitive circuits. Brain Res Brain Res Rev 31: 236–250 .
- Dum RP, Strick PL (2002) Motor areas in the frontal lobe of the primate. Physiol Behav 77: 677–682.
- Dum RP, Strick PL (2005) Frontal lobe inputs to the digit representations of the motor areas on the lateral surface of the hemisphere. J Neurosci 25: 1375–1386.
- Dieterich M, Bucher SF, Seelos KC, Brandt T (1998) Horizontal or vertical optokinetic stimulation activates visual motion-sensitive, ocular motor and vestibular cortex areas with right hemispheric dominance: An fMRI study. Brain 121: 1479-1495 .
- Bense S, Janusch B, Vucurevic G, Bauermann T, Schlindwein P, et al. (2006) Brainstem and cerebellar fMRI-activation during horizontal and vertical optokinetic stimulation. Exp Brain Res 174: 312-323 .
- Mercier L, Audet T, Hebert R, Rochette A, Dubois M (2001) Impact of motor, cognitive and perceptual disorders on ability to perform activities of daily Living after stroke. Stroke 32: 2602-2608 .
- Verheyden G, Nieuwboer A, De Wit L, Feys H, Schuback B, et al. (2007)Trunk performance after stroke: an eye catching predictor of functional outcome. J Neurol Neurosurg Psychiatry 78: 694–698 .
- Oliveira CB, Medeiros ÍR, Greters MG, Frota NA, Lucato, LT, et al. (2011) Abnormal sensory integration affects balance control in hemiparetic patients within the first year after stroke. Clinics [Sao Paulo] 66: 2043-2048.
- Angelaki DE, Cullen KE (2008) Vestibular System: The Many Facets of a Multimodal Sense. Annu. Rev. Neurosci 31: 125–150.
- Chen H-C, Dromerick AW, Edwards DF (2011) Very early constraints-induced movement therapy [VECTORS]: Effects of timing or dose on upper extremity function. Archives of Physical Medicine and Rehabilitation 92: 1701-1702.
- (2012) Intercollegiate Stroke Working Party. National clinical guideline for stroke, 4th edition. London: Royal College of Physicians;
-
-









Table 1:
Participant selection criteria.