Authors:
Sanou Sobze Martin1, Djeunang Dongho Ghyslaine Bruna1*, Russo Gianluca2, Zefack Yannick3, Sali Ben Bechir Adogaye1, Tsi Kien-Atsu1, Fotso Jimmy Roger1, Tiotsia Tsapi Armand1, Ercoli Lucia3, Colizzi Vittorio4 and Zambou Ngoufack Francois5
1Department of Biomedical Sciences, Faculty of Science, University of Dschang, PO Box 67 Dschang, Cameroon.
2Department of Infectious and Tropical Diseases, University of Rome “La Sapienza”, Italy
3Soledale Medical Institute (IMES), Rome, Italy
4Department of Experimental Medicine, biological and biochemical sciences, University of Roma “Tor vergata”, Italy
5Laboratory of Biochemistry, Nutrition and Food Sciences (LABPMAN), Department of Biochemistry, Faculty of Science, University of Dschang. PO Box 67 Dschang, Cameroon
Received: 12 January, 2014; Accepted: 30 March, 2015; Published: 31 March, 2015
DJEUNANG Dongho Ghyslaine Bruna, University of Dschang, PO Box 67 Dschang, Tel: (+237) 694543116/674495408; Email:
Martin SS, Ghyslaine Bruna DD, Gianluca R, Yannick Z, Bechir Adogaye SB, et al. (2015) Nutritional outcomes in HIV-Exposed Infants in the Mingha Program, Dschang-Cameroon (2003-2011). J HIV Clin Scientific Res 2(1): 016-022. DOI: 10.17352/2455-3786.000009
© 2015 Martin SS, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Nutritional outcomes; HIV-exposed children; Mingha program; Dschang; Cameroon
ANOVA: Analysis of Variance; ARV: Antiretrovirals; ANC: Antenatal Care; DHD: Dschang Health District; EDS-MICS: Demographic and Health Survey Multiple Indicator; GSK: “GlaxoSmithKline”; NIS: National Institute of Statistics; MINSANTE: Ministry of Public Health; NIAID: “National Institute of Allergy and Infectious Disease”; MDGs: Millennium Development Goals; WHO: World Health Organization; UN: United Nations; UNAIDS: United Nations Joint Program on HIV / AIDS; PCR: “Polymerase Chain Reaction”; PIPAD: Projet Intergre pour la Promotion de l'Aauto Developement; PMTCT: Prevention of Mother to Child Transmission; PLWHIV: People Living with HIV; AIDS: Acquired Immunodeficiency Syndrome; SPSS: “Statistical Package for Social Science”; ART: Antiretroviral treatment; MTCT: Mother to Child Transmission; UNGASS: “United Nations General Assembly Special Session on HIV and AIDS”; UNICEF: United Nations Children's Emergency Fund; USBC: “United States Breastfeeding Commitee”; HIV: Human Immunodeficiency Virus; HIV +: Positive for HIV testing; Z-BMI: Z-score of Body Mass Index; Z-LA: Z-score Length for Age; Z-WA: Z-score Weight for Age; Z-WL: Z-score weight for length
Background: Prevention of Mother to Child Transmission (PMTCT) is a set of interventions that contribute in reducing the risk of HIV transmission from mother (parents) to the child. The infant feeding choice in the HIV context remains a key item of PMTCT. This study aimed at evaluating the nutritional status of children followed by the Mingha / PMTCT program in the Dschang Health District (DHD) during 09 years of activities. We used a descriptive study based on retrospective data from an intervention conducted at the DHD between 2003 and 2011 on a group of mother-child pairs in the PMTCT (Mingha/PMTCT) facilitation program. The intervention was the formula feeding given to the children from birth till 18 months. The data collected was analyzed using SPSS Version 18 software.
Results: Among 328 children accessed, we had a sex ratio of 0.83 with more boys than girls. Severe wasting was found only within 11 boys (3.26%) and only <6 months old children were concerned. Moderate wasting was found among 6 girls (1.74%) and 5 boys (1.52%) and <6 months old children were highly concerned 10 (3.17%). Overweight (3.26%) was highly predominant among 8 boys (2.24%) and except those of <6 months, all the other age groups were concerned. There were no cases of obesity or stunting.
Conclusions: The nutritional status of the Mingha/PMTCT program children was quite satisfactory. It characterizes the hope for a suitable nutritional follow up of children in HIV context. Therefore programs like Mingha/PMTCT should be promoted and transferred to other Health Districts and even resource-limited Countries.
Background
According to reports of the United Nations, the Human Immunodeficiency Virus (HIV) is the leading cause of mortality and morbidity in women of reproductive age worldwide [1]. In Cameroon, the prevalence of HIV infection in pregnant women ranges from 5 to 18% depending on the region [2]. According to the UNGASS 2010 UNAIDS report, the average rate of vertical transmission in Cameroon is 19%. However, a study conducted at the Douala General Hospital over a period of 6 years (January 2002-December 2007) on pregnant women who received antenatal care (ANC) showed a prevalence of HIV seropositivity of 2.62%. This figure was justified by the standard of that hospital that received women with medium or high socioeconomic level [3].
Prevention of Mother to Child Transmission (PMTCT) is a set of interventions that contribute in reducing the risk of HIV transmission from mother (parents) to child. HIV transmission from mother to child can be realized without prevention in 25-40% of cases, especially during pregnancy (20%), at the time of delivery (65%) or during the period of breastfeeding (15%) [4]. Mother to Child Transmission (MTCT) is the most important route of HIV infection among children aged less than 15 years [5]. PMTCT which is the most important strategy in the management of HIV/AIDS infection remains a “challenge” in most resource-limited countries, particularly in Africa [6].
The type of feeding subjected to children born in the context of HIV remains controversial. When PMTCT was initiated in Cameroon, the type of feeding recommended was formula feeding. This was due to the fact that, cases of transmission of HIV from mother to child identified were attributable to unsafe breastfeeding [7,8]. Today, breastfeeding alongside taking ARVs is recommended to women during ANC as a reason for the presence of immune hedges in breast milk [9-13]. However, the systematic use of tri-therapy remains the ideal solution because it decreases the risk of vertical transmission below 2% or 1% [12,14-18]. According to the World Health Organization (WHO), the implementation of treatment guidelines to reduce the risk of MTCT to less than 5% in populations practicing breastfeeding (with the baseline risk of 35%) and less than 2% in those not practicing breastfeeding (where the baseline risk of 25%) [19].
The Mingha/PMTCT project was initiated and developed in 2003 by the Italian Association Mingha Africa Onlus in collaboration with the PIPAD (Projet integré pour la promotion de l'auto-développement) in the Dschang Health District (DHD) and its surroundings. Mingha, a word borrowed from the “Yemba” dialect means ‘my child'. It is a PMTCT facilitation project in rural areas. It dealt with women opting for formula feeding according to the PMTCT guidelines put in place in Cameroon between 2003 and 2011. In this project, the mother-child pairs were given nutritional support in terms of formula feeding, tips for a healthier lifestyle, help in adherence to ARV treatment for the women eligible, and medical follow up.
Cameroon still faces Antiretroviral (ARV) availability problems for treatment of people living with HIV (PLWHIV) and tri-therapy in the context of PMTCT till date [20]. For these reasons, formula feeding remains among others the most powerful options for the newborn. It would be beneficial for stakeholders of the health system to know the benefits of nutritional monitoring. This is what justifies this study.
Materials and Methods
Study design
We proceeded by a retrospective descriptive study based on data previously collected from an intervention conducted on several mother-child pairs whose mothers were HIV +. This study was done in the context of PMTCT facilitation, with the help of mothers regarding child nutrition by grants of formula feeding to children from birth till 12 months of age associated with practical tips for a better quality of life as PLWHIV as well as therapy adherence within the Mingha/PMTCT project within 09 years (2003-2011).
Site and study period
The Dschang Health District consists of 22 health areas grouped into three, Urban, suburban and rural. In this Health District, almost all tribes and religions of Cameroon are represented. This study was extended from December 2013 to March 2014. In the month of February 2014, the collected was analyzed within the premises of the PIPAD development association through its Mingha/PMTCT program whose actions cover the entire district. The starting point was the District Hospital of Dschang where all the women were recruited and followed after giving birth until the children were 18months old. The mapping of this area is presented in Figure 1.
Sampling: The present study lasted for 9 years (2003-2011) and had a cohort nature. The target sample was HIV exposed children i.e. children born from HIV+ mothers. A two stage exhaustive sampling was used. The first stage included all the HIV + mothers followed under Mingha/PMTCT program and the second stage was the selection of infants from all the chosen mothers. This gave us in total 324mothers with 328 children since there were 4pairs of twins.
• Anthropometric measurements Weight measurement: It was done once every month during visits to the medico-social centre of PIPAD with a baby scale of brand SECA.
Before weighing, the scale was calibrated using the same standard (comfortable).
The weighing procedure was as follows; the naked child lay or sat in the tray, the latches were displaced (kg prior to that of grams) until the control bar was balanced then the nurse read and recorded the weight of the latter.
• Length measurement: It was done once every month during visits to the medico-social center of PIPAD using a tape.
While taking the size, the child could stand, was dressed, barefoot, standing straight, arms along the body, head and shoulders upright.
The nurse in charge of reading and noting the parameter stood in front of the child, took a straight look perpendicular to the height guage and the upper limit of the head of the child.
Regarding infants and babies, their sizes were taken using a measuring tape. During measurement, they were held by the feet, head down, and the measurements were taken from the heels to head.
• HIV screening in children: it was done at the medico-social center of PIPAD. Blood specimens of the children under the cautious watch of their mothers were collected at the anterior face of the elbow or the jugular vein (neck) or ankle (behind the external malleolus), using a 5 ml syringe for 18 months old children. Blood collected was then put in a dry tube and centrifuged. The serum produced was put on a strip for quick test. The results were read by a practitioner after 5 to 15 minutes according to the following nomenclature: one bar (negative serology), two bars (positive serology).
Intervention/nutritional support
The interventions benefited by mother-child pairs at the PMTCT (Mingha/PMTCT) facilitation program, consisted essentially of nutritional support for children on formula feeding in proportions depending on the age that is specified in the document entitled Annex 1 Table showing the distribution of milk according to age in the Mingha/PMTCT project.
Statistical analysis
For the determination of sample characteristics, we used the usual statistics. That is, the mean, standard deviation (SD) and percentage (ratio).
For the evaluation of the nutritional status of children, Z-scores were used. These were the Z-WL (Z-score weight for length), Z-LA (Z-score Length for Age), Z-WA (Z-score Weight for Age), Z-BMI (Z-score of Body Mass Index). They allow a better assessment of the various degrees of malnutrition, whether acute or chronic malnutrition as well as wasting, stunting, overweight and obesity. We used the variance analysis test (ANOVA) for comparing the Z-scores for children to each meeting.
The significant threshold selected for all these analyses was 0.05. Statistical analysis was performed using SPSS Version 18 software.
Results
Sample Characteristics
For this study, a total of 376 children were followed. Of these, we recorded 06 children whose mothers were false positive for HIV screening, 29 children whose mothers' records were incomplete and did not allow us to have any data on the birth of the child, and 13 children whose mothers (were not HIV positive) had some health problems, had died or were indigent. We were finally left with 328 children whom we selected for the study. These children were followed from 2003 to 2011 with 3439 passages at the Medico-Social Centre of PIPAD. On average 10.29 passes per child for a minimum of 1 pass and a maximum of 34 passes were recorded. Of the 328 children, 149 or 45.4% were girls and 179 or 54.6% were boys for a sex ratio of 0.83. The frequency of recruitment by sex per year of the children followed presented in Figure 2 allowed us to note that the largest number of recruitment was done in 2007 that is 52 children (15.8%) against a lower number of recruitment in 2003, 14 children (4.3%).
-
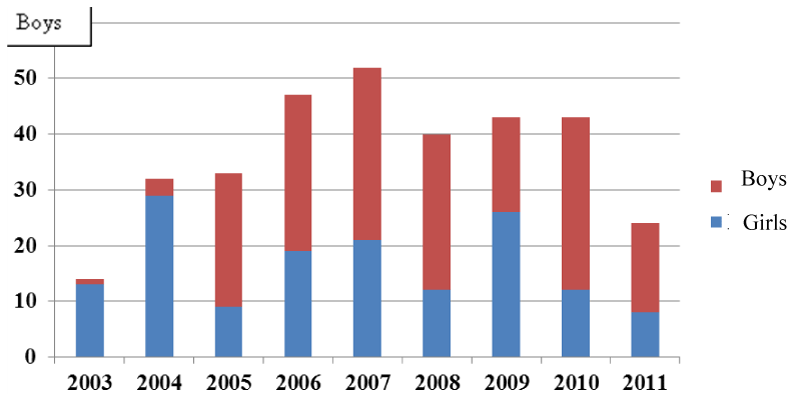
Figure 2
Distribution of children by sex and year of monitoring in Mingha / PMTCT program.
The average birth weight of 315 children for whom this variable was available was 2996.80 grams (g) with a minimum of 1,350 g and a maximum of 4,500 g and a standard deviation of 519.286g.
The distribution of birth weight during the years of follow up as presented in Figure 3 found that 50 children (15.9%) had a low birth weight, 258 children (81.9%) had a normal birth weight and 7 children (2.2%) had a birth weight above the normal or were big babies.
It is clear from Table 1 that there is no correlation between birth weight and sex of the children followed since the P value> 0.05. In other words, birth weight does not depend on gender. The vast majority of children (81.9%) have a normal birth weight, while 15.9% have low birth weight.
1. Nutritional status of children followed
Of the 328 children followed, 90.6% were fed by formula feeding from birth; 9.1% to breastfeeding and 0.4% mixed feeding. Those children who were entitled to breastfeeding had an average duration of lactation of 9.78 weeks for a minimum of 2 weeks and a maximum of 24 weeks with a standard deviation of 7.34 weeks.
Table 2 shows that only boys (3.26%) suffered from severe acute malnutrition. Meanwhile girls were more prone to moderate acute malnutrition (1.74%) than boys (1.52%). In general, 4.78% of the boys followed in the project Mingha suffered from acute malnutrition, while 1.74% of girls suffered the same effect. No cases of stunting and underweight were recorded.
-

Table 1:
Relation between sex and birth weight.
Pearson chi2 (2) = 2.3821 P-value = 0.304
Table 3 reveals that the age group of less than 6 months was affected by severe acute and moderate malnutrition with prevalences of 3.26% and 3.17% respectively. However, it is not the only age group affected as those of 6 to 11 months were also subject to moderate malnutrition (0.09%). In general, 6.43% of children less than 6months and 0.09% of children 6 to 11 months suffer from acute malnutrition. The age groups from 12 to 17 months and 18 months and did not record any malnutrition problems.
Regarding overweight and obesity, no obesity was detected as against some cases of overweight present. Table 4 gives precise figures. It shows that both sexes were affected, 1.02% in girls and 2.24% in boys. All ages, except those less than 6 months were affected. The prevalence of overweight among 6-11 months, 12-17 months and over 18 months were respectively 1.31%, 1.74% and 0.21%.
Anthropometric parameters of the children followed were compared by passing to verify the existence of any significant difference between the various passage indices. The test results of one-way ANOVA performed is in Table 5 shows that there was a highly significant difference between the intergroup variability and intra-group variability in each of the monitoring of these children indexes. So there is a difference between children of monitoring parameters on each pass.
Discussion
Several studies assessing the nutritional status of children exist in the world and Cameroon. Very few of them were conducted to specifically assess the nutritional status of children born to HIV positive mothers and more with an objective of evaluating a health program in a health district. Some studies assessed the nutritional status of pre-school children and sometimes mothers living with HIV who gave birth.
The Mingha program recruited 328 children after 9 years of activity with a male predominance (54.6%). In this group of children, malnutrition was felt very little. Moderate acute malnutrition affected 1.52% of the male population with 3.26% severe acute malnutrition recorded mainly in boys. Furthermore, being overweight was detected in 3.26% of the population only. In general, the children followed in the Mingha / PMTCT program physically normally developed.
The year in which the largest number of recruitment was done was 2007 (15.8%). The explanation is that the Mingha program was sufficiently popularized and known from this period in the DHD. 15.9% of children followed had birth weight below 2500g. This rate was higher than that found in the Cameroonian population (10%) in 2011 EDS-MICS [21]. It could be due to the clinical status of their mothers rather than their unstable HIV-positive status. Their birth weight was shown not to depend on their sex according to the P-value of Table 1. The nature of the study could not permit us have clear explanation on the link between the birth weight and sex since many factors were supposed to be included in the evaluation [22].
The anthropometric measures of children followed in the Mingha/PMTCT project were better than those of children born to healthier mothers and those of children in some localities of Cameroon and the world. This study showed a moderate acute malnutrition rate of 3.26% with a female predominance (1.74%), severe acute malnutrition rate of only 3.26% in boys and overweight rate of 3.26% with a male predominance (2.24%). These figures are close to those found by Chiabi Andreas et al. in Yaounde HGOPY in a group of apparently healthy children [23]. They are slightly low compared to those obtained by Owona in 2001, Ateba Emvoutou in 2006 and Nem Tchuenteu in 2009 among children attending schools [24-26]. This could be due to the children's recruitment site which is the school, where the child is usually easily devoid of parental attention regarding food. These figures are very low compared to those reported by Motouom studies in 2004 at Mingao in Yaoundé and Betsem in 2001 at Niété in the South Region [27,28]. This could be explained by the place of recruitment which is the community where we meet children from all backgrounds and from families with different incomes. There are also the places where there is food insecurity due to the lack of agricultural diversity and availability in sufficient quantities of these foods. Monitoring the parameters of children during each contact (Meeting at health center of PIPAD) were statistically different, and this significantly sticks to the result of the ANOVA test, which reinforces the idea that the nutritional support to children benefits them.
This study is a particular approach regarding the investigation for the fight against HIV / AIDS and the Millennium Developmental Goals (MDGs). Its main limitation is the fact that investigators were not able to verify the effectiveness of the adequate intake of milk, which was awarded to the child. In addition, the sample size and the place of recruitment of mother-child pairs followed (District Hospital Dschang) which is the central point of health care of PLWHIV in the DHD do not give us the ability to infer results in the DHD. To these two elements, we can add the fact that in the DHD mother-child pairs in context HIV could be followed elsewhere.
Conclusion
The purpose of this study was to assess the Mingha / PMTCT program's impact on the nutritional status of children born to HIV + mothers in the DHD during 09 years of activity. At the end of it, it appears that only boys were affected by severe wasting (3.26%), while both sexes were affected by moderate wasting with a female predominance (1.74%). In addition, the most affected by wasting were less than 6 months of age (3.26%). No cases of stunting or obesity were recorded. The Mingha program produced satisfactory results regarding nutritional outcomes. Such results show the hopeful possibility of a “generation without AIDS” despite the difficulties of access to ART. Formula feeding remains a possibility for actions that should not be overlooked in the context of the fight against HIV.
Acknowledgment
Sincere gratitude goes to the mother-child pairs who agreed to participate in the Mingha/PMTCT Program. Our gratitude also goes to the different authors of this article for their particular contributions as follows:
DD conceived the paper, contributed to data interpretation and validation, drafted manuscript and submitted the manuscript; SS participated in study protocol development and definition of objectives and reviewed several versions of the manuscript; RG collected data, participated in study protocol development and definition of objectives and revised the manuscript critically for important intellectual content; ZY reviewed several versions of the manuscript; SB reviewed several versions of the manuscript; TK-A revised the manuscript critically for important intellectual content; FJ reviewed several versions of the manuscript; TT reviewed several versions of the manuscript; EL revised the manuscript critically for important intellectual content; VC revised the manuscript critically for important intellectual content; ZN participated in study protocol development and definition of objectives and revised the manuscript critically for important intellectual content.
We also thank Mr AMADOU Salmon who helped us in analyzing data and the team work of the Mingha program for recruiting mother and child pairs and doing the follow up. It will be a huge mistake to complete this section without acknowledging our partners Mingha Africa Onlus, Tavola Valdese and IMES.
-

Annex 1:
Table showing the distribution of milk according to age in the Mingha / PMTCT project.
- ONU (2009) Les femmes et la sante. In : Rapport de l'Organisation des Nations Unies.
- Fondation GSK (2008) Prevention du risque de transmission du VIH de la mère à l'enfant au Cameroun.
- Tsingaing KJ, Egbe OT, Halle EG, Tchente NC, et al. (2011) Prevalence du VIH chez la femme enceinte et transmission mère-enfant du VIH à la maternite de l'Hôpital General de Douala, Cameroun, Clinics in Mother and Child Health, 8(C100801), 3 p.
- MINSANTE (2011) Formation des prestataires sur les nouvelles directives PTME et option d'alimentation infantile en contexte VIH au Cameroun, 131p.
- UNICEF (2004) WCARO Cameroon pub KitPTME. Generalites sur la PTME, Fiche2, pp.3.
- Becquet R, Ekouevi DK, Arrive E, Stringer JS et al. (2009) Universal antiretroviral therapy for pregnant and breast-feeding HIV-1-infected women: towards the elimination of mother-to-child transmission of HIV-1 in resource-limited settings. Clin Infect Dis 49: 1936-1945.
- Prebbe E, Piwoz EG (1998) HIV and Infant Feeding: A Chronology of Research and Policy Advances and their Implications for Programs.
- Magoni M1, Bassani L, Okong P, Kituuka P, Germinario EP, et al. (2005). Mode of infant feeding and HIV infection in children in a program for prevention of mother-to-child transmission in Uganda. AIDS 19: 433-437.
- Latham MC, Prebbe EA (2000) Appropriate feeding methods for infants of HIV infected mothers in sub-Saharan Africa. BMJ 320: 1656-1660.
- Stuebe A (2009) The risks of not breastfeeding for mothers and infant. Rev Obstet Gynecol 2: 222-231.
- USBC (2011) Breastfeeding a vision for the future, supporting families: Improving health.
- Young SL, Mbuya MN, Chantry CJ, Geubbels EP, Israel-Ballard K, et al. (2011) Current Knowledge and Future Research on Infant Feeding in the Context of HIV: Basic, Clinical, Behavioral, and Programmatic Perspectives. Adv Nutr 2: 225-243.
- Liamputtong P, Sulaiman Z, Amir L (2011) Infant feeding practices: Rates, Risks of Not Breastfeeding & Factors Influencing Breastfeeding, University La Trobe.
- NIAID (2000) Fact sheet: HIV infection in women, National Institute of Health, Bethesda, MD, USA, November.
- Becquet R (2009) Les nouvelles orientations de la Prevention de la Transmission Mère-Enfant du VIH (PTME) en Afrique. In : 10e Journee nationale d'Infectiologie, juin 2009, Lyon.
- Russo G, Lichtner M, Traditi F, Vullo V (2009) Is the time for an AIDS-free new generation different in resources-limited and industrialized countries? AIDS 23: 293-296.
- Simpkins EP, Siberry GK, Hutton N (2009) Thinking about HIV infection. Pediatr Rev 30: 337-349.
- Reshi P, Lone IM (2010) Human immunodeficiency virus and pregnancy. Arch Gynecol Obstet 281: 781-792.
- WHO (2010) PMTCT strategic vision 2010-2015: preventing mother-to child transmission of HIV to reach the UNGASS and Millennium Development Goals.
- Alyos E. (2013) SIDA/VIH: penurie d'antiretroviraux au cameroun, Fil Rouge [online].
- INS (2011) Enquête Demographique de Sante à Indicateurs Multiples, 546p.
- Bii SC, Otieno-Nyunya B, Siika A, Rotich JK (2008) Infant feeding practices among HIV infected women receiving prevention of mother-to-child transmission services of Kitale District Hospital, Kenya. East Afr Med J 85: 156-161.
- Chiabi A, Tchokoteu PF, Takou V, Fru F, Tchouine F (2008) Anthropometric measurements of children attending a vaccination clinic in Yaounde, Cameroon. Afr Health Sci 8: 174-179.
- Owona M (2001) Obesite et equilibre energetique chez l'enfant en milieu scolaire à Yaounde. Thèse de doctorat d'État en Medecine, Universite de Yaounde I, Faculte de Medecine et des Sciences Biomedicales.
- Ateba ETS (2006) Évaluation du statut nutritionnel et anemique chez les enfants infestes par les mesoparasites dans deux ecoles maternelles (urbaine et peri urbaine) de la ville de Yaounde. Memoire en vue de l'obtention du Diplôme de Technicien Medico-Sanitaire, Centre d'Enseignement Specialise des Techniques d'Analyses Medicales (CESTAM).
- Nem TD (2009) Donnees anthropometriques des enfants d'âge prescolaire à Garoua, Cameroun [online]. Memoire pour Diplôme de specialiste en pediatrie, Universite de Yaounde I, Faculte de Medecine et des Sciences Biomedicales.
- Betsem a Betsem E (2001) Évaluation de l'etat nutritionnel des enfants de 6 à 60 mois dans la localite de Niete. Thèse de doctorat d'État en Medecine, Universite de Yaounde I, Faculte de Medecine et des Sciences Biomedicales.
- Motouom G (2005) Évaluation de l'etat nutritionnel des enfants de moins de 5 ans d'un quartier de niveau socio-economique bas et moyen de Yaounde. Thèse de doctorat d'État en medecine, Universite de Yaounde I, Faculte de Medecine et des Sciences Biomedicales.




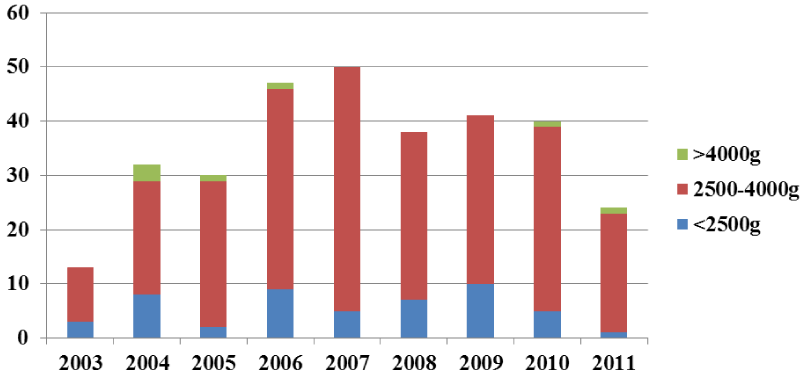





Figure 1
Localisation of Dschang Health District and surroundings.
Figure 1
Localisation of Dschang Health District and surroundings.